-
摘要: 目的 腹腔镜手术因取出标本而留下的手术瘢痕,影响到切口美容效果,导致切口周围感觉、运动障碍。单切口经脐三角腹腔镜(single-incision triagulated umbilicus surgery,SITUS)技术已成功应用于多种腹部外科手术,与传统腹腔镜技术相比,在皮肤美容效果上具有优势,操作便利度和学习曲线基本相同。本研究旨在总结150例SITUS手术患者的临床资料,探讨SITUS技术在腹腔脏器切除手术的可行性、安全性。方法 回顾性分析2015年8月—2020年9月我院实施的150例SITUS泌尿外科手术,总结分析手术时间、术中失血量、术后留置引流管时间、术后住院天数、患者瘢痕评估问卷(PSAQ)评分等临床数据。结果 150例手术均顺利完成,无中转开放手术或传统腹腔镜手术,所有手术标本自脐部新月形切口拉伸后取出。腹腔内手术结束后,向心性缝缩切口,术后美容效果满意。围手术期未发生Clavien Ⅲ级以上并发症。结论 SITUS手术方式进行腹盆腔脏器切除手术安全可行,术后瘢痕可隐藏于脐周围。尤其对于大体积标本切除患者,SITUS除了具有美容优势,还具有功能恢复上的优势。Abstract: Objective The surgical scar caused by conventional laparoscopic surgery may affect the cosmetic effect and cause sensory and motor disorders. Laparoscopic single incision triangulated umbilicus surgery (SITUS) has been successfully applied in many abdominal surgeries, which showed the advantages of the cosmetic effect over conventional laparoscopy with almost equal operative difficulty and equal learning curve. The purpose of this study is to summarize the clinical data of 150 cases of SITUS and to investigate the feasibility and safety of SITUS.Methods From August 2015 to September 2020, 150 cases of SITUS with organ resection were performed, and clinical data were analyzed retrospectively. The clinical data such as operation time, estimated blood loss, postoperative drainage tube time, postoperative hospital stay and PSAQ score were analyzed.Results All 150 procedures were successfully completed without conversion to open surgery or conventional laparoscopic surgery. All surgical specimens were removed from the crescent incision around the umbilicus. After suturing the incision, the cosmetic effect was satisfactory, and no patients suffered complications greater than or equal to Clavien Grade Ⅲ.Conclusion SITUS is safe and feasible for large abdominal and pelvic organ resection operations. The incision scar can be hidden in the edge of umbilicus.SITUS not only has the advantages of cosmic effect, but also has the advantages of functional recovery, especially for patients with large specimens.
-

-
表 1 手术经验对围手术期各项指标的影响
X ± S 指标 总90例 前20例 后70例 P值 失血量/mL 67.28±26.22 62.25±25.62 68.71±26.21 >0.05 手术总时间/min 106.83±19.29 113.50±14.33 104.93±20.08 >0.05 腹腔内操作时间/min 71.11±15.52 73.75±9.86 70.36±16.72 >0.05 开关切口时间/min 35.72±7.09 39.75±6.61 34.57±6.80 < 0.01 输血/例 0 0 0 - 住院时间/d 3.96±0.76 4.15±0.85 3.90±0.72 >0.05 拔除引流管时间/h 65.02±13.01 69.70±15.40 63.69±11.90 >0.05 PSAQ评分/分 60.71±11.13 72.50±7.76 57.34±9.54 < 0.01 VAPS疼痛评分/分 0.67±0.70 0.65±0.65 0.67±0.71 >0.05 表 2 术后相关并发症
术后并发症 等级 例数 处理 发热 Ⅰ 5 保守治疗 疼痛 Ⅰ 10 口服止痛药 皮下气肿 Ⅰ 1 保守治疗 尿潴留 Ⅰ 3 导尿 出血 Ⅱ 1 输血 伤口感染 Ⅱ 2 换药、抗感染治疗 深静脉血栓 Ⅱ 1 药物治疗 肺炎 Ⅱ 1 药物治疗 肺水肿 Ⅲ 0 - 肠穿孔 Ⅲ 0 - 心梗 Ⅳ 0 - 死亡 Ⅴ 0 - -
[1] Fink C, Baumann P, Wente MN, et al. Incisional hernia rate 3 years after midline laparotomy[J]. Br J Surg, 2014, 101(2): 51-54.
[2] Nagele U, Walcher U, Herrmann TR. Initial experience with laparoscopic single-incision triangulated umbilical surgery(SITUS)in simple and radical nephrectomy[J]. World J Urol, 2012, 30(5): 613-618. doi: 10.1007/s00345-011-0670-7
[3] 祝广峰, 窦小亮, 郑小龙, 等. 经脐可拉伸切口腹腔镜术式在大肾癌切除术中的应用体会[J]. 现代泌尿外科杂志, 2017, 22(6): 433-436. doi: 10.3969/j.issn.1009-8291.2017.06.008
[4] 张雪培. 泌尿外科腹腔镜手术图解[M]. 郑州: 河南科技出版社, 2014: 44-58.
[5] 祝广峰, 窦小亮, 张志明, 等. 单切口经脐三角腹腔镜手术在右侧肾上腺肿瘤切除中的初步应用[J]. 现代泌尿外科杂志, 2017, 22(11): 844-847. doi: 10.3969/j.issn.1009-8291.2017.11.010
[6] 祝广峰, 窦小亮, 付强, 等. 单切口经脐三角腹腔镜与传统经腹腹腔镜在肾切除中的应用比较[J]. 现代泌尿外科杂志, 2018, 23(10): 759-764. doi: 10.3969/j.issn.1009-8291.2018.10.010
[7] Horstmann M, Kugler M, Anastasiadis AG, et al. Laparoscopic radical cystectomy: initial experience using the single-incision triangulated umbilical surgery(SITUS)technique[J]. World J Urol, 2012, 30(5): 619-624. doi: 10.1007/s00345-012-0909-y
[8] 窦小亮, 汪涌, 陈晓鹏, 等. 经脐单切口三角位腹腔镜技术在腹膜外膀胱部分切除术中的应用[J]. 现代泌尿外科杂志, 2020, 25(9): 793-797. doi: 10.3969/j.issn.1009-8291.2020.09.007
[9] 许景洪, 李立志, 黄文文, 等. 腹部腹腔镜手术后大块标本取出的切口并发症的多因素分析[J]. 中国微创外科杂志, 2014, 14(9): 792-795. doi: 10.3969/j.issn.1009-6604.2014.09.007
[10] Pelosi MA, Pelosi MA 3rd. Laparoscopic appendectomy using a single umbilical puncture(minilaparoscopy)[J]. J Reprod Med, 1992, 37(7): 588-594.
[11] 徐辉, 张国玺, 邹晓峰, 等. 耻骨上辅助单孔腹腔镜上尿路全切术四例报告[J]. 中华医学杂志, 2019, 99(36): 2840-2843.
[12] 陈琳, 郑莹, 闵玲, 等. vNOTES与TU-LESS行子宫全切除术的临床队列研究[J]. 中华妇产科杂志, 2020, 55(12): 843-847. doi: 10.3760/cma.j.cn112141-20200309-00193
[13] 王林辉, 吴震杰, 朱清毅. 中国泌尿外科单孔腹腔镜技术的发展与展望[J]. 中华泌尿外科杂志, 2020, 41(11): 807-810. doi: 10.3760/cma.j.cn112330-20200925-00684
[14] 邓仲磊, 苏学林, 苏健, 等. 经脐单孔腹腔镜联合经尿道途径辅助单侧肾输尿管全长逆行切除术的可行性及安全性分析[J]. 中华泌尿外科杂志, 2020, 41(11): 820-824. doi: 10.3760/cma.j.cn112330-20200407-00272
[15] Autorino R, Cadeddu JA, Desai MM, et al. Laparoendoscopic single-site and natural orifice transluminal endoscopic surgery in urology: a critical analysis of the literature[J]. Eur Urol, 2011, 59(1): 26-45. doi: 10.1016/j.eururo.2010.08.030
[16] 刘青, 关小明. 单孔腹腔镜在妇科中的应用现状及发展[J]. 实用妇产科杂志, 2019, 35(3): 161-163. https://www.cnki.com.cn/Article/CJFDTOTAL-SFCZ201903002.htm
[17] 黄琳娟, 代雪林, 唐均英, 等. "三位一体"认识和处理单孔腹腔镜的"筷子效应"[J]. 医学与哲学, 2018, 39(18): 76-77, 86. https://www.cnki.com.cn/Article/CJFDTOTAL-YXZL201809024.htm
[18] Cao J, Liu B, Li X, et al. Analysis of delayed discharge after day-surgery laparoscopic cholecystectomy[J]. Int J Surg, 2017, 40: 33-37. doi: 10.1016/j.ijsu.2017.02.055
[19] Wolters M, Imkamp F, Wohlatz L, et al. Laparoendoscopic partial nephrectomy in single-incision triangulated umbilical surgery(SITUS)technique: early experience[J]. World J Urol, 2015, 33(3): 403-412. doi: 10.1007/s00345-014-1320-7
[20] Schoenthaler M, Avcil T, Sevcenco S, et al. Single-Incision Transumbilical Surgery(SITUS)versus Single-Port Laparoscopic Surgery and conventional laparoscopic surgery: a prospective randomized comparative study of performance with novices in a dry laboratory[J]. World J Urol, 2015, 33(1): 51-57. doi: 10.1007/s00345-014-1266-9
[21] 汪涌, 祝广峰, 窦小亮, 等. 改良经脐单切口三角腹腔镜在肾盂癌根治术中的首次应用(附4例报告)[J]. 临床泌尿外科杂志, 2017, 32(9): 695-697, 702. https://www.cnki.com.cn/Article/CJFDTOTAL-LCMW201709012.htm
[22] Durani P. Patient assessments of scarring: patient-reported impact of scars measure or patient scar assessment questionnaire?[J]. Plast Reconstr Surg, 2011, 127(4): 1744-1745. doi: 10.1097/PRS.0b013e31820a667c
-

| 引用本文: | 祝广峰, 窦小亮, 余雨豪, 等. 单切口经脐三角腹腔镜150例手术经验总结[J]. 临床泌尿外科杂志, 2022, 37(1): 20-24. doi: 10.13201/j.issn.1001-1420.2022.01.005 |
| Citation: | ZHU Guangfeng, DOU Xiaoliang, YU Yuhao, et al. Experience of single incision triangulated umbilicus surgery in 150 cases[J]. J Clin Urol, 2022, 37(1): 20-24. doi: 10.13201/j.issn.1001-1420.2022.01.005 |
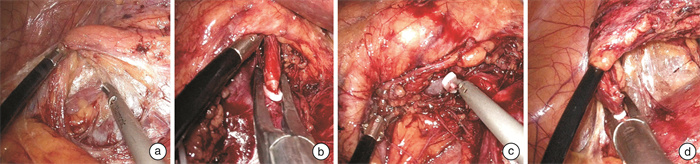
- Figure 1.
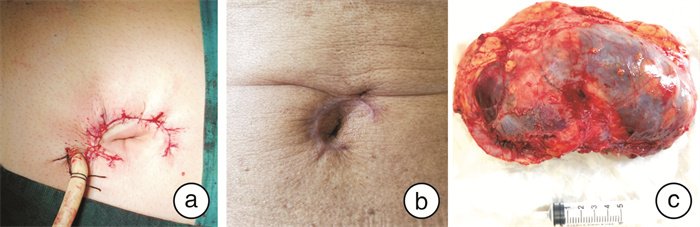
- Figure 2.
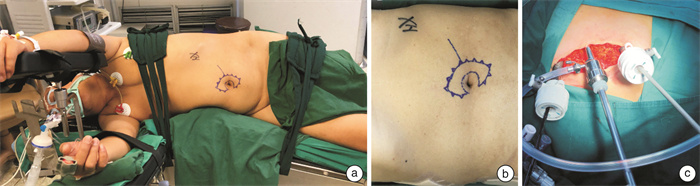
- Figure 3.



 下载:
下载: