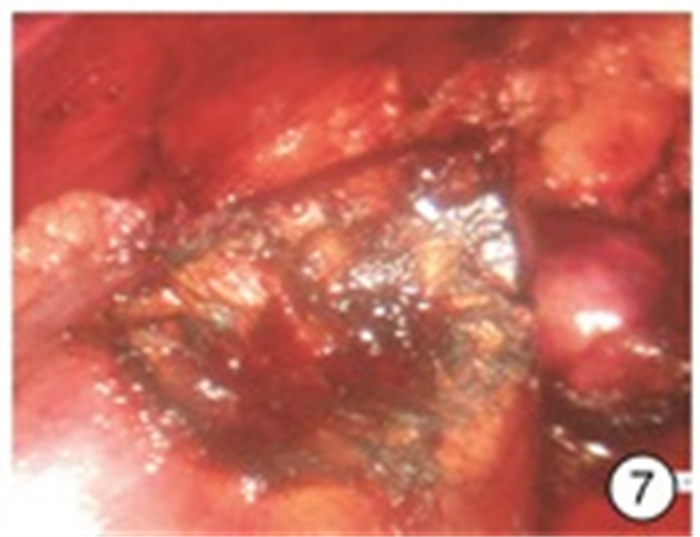
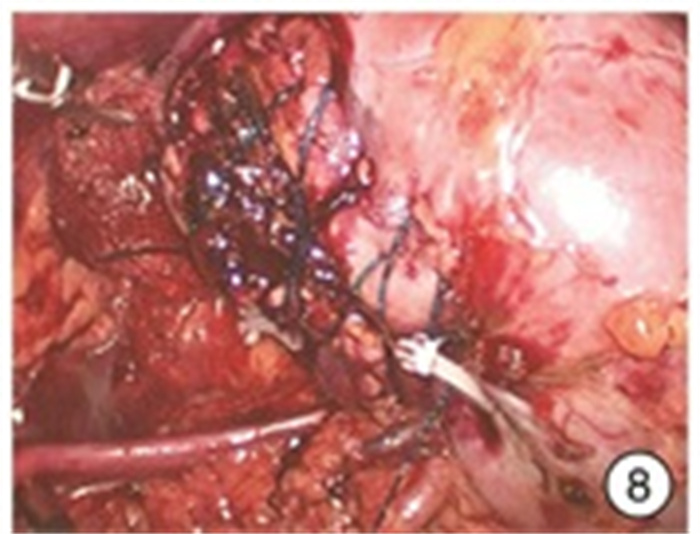
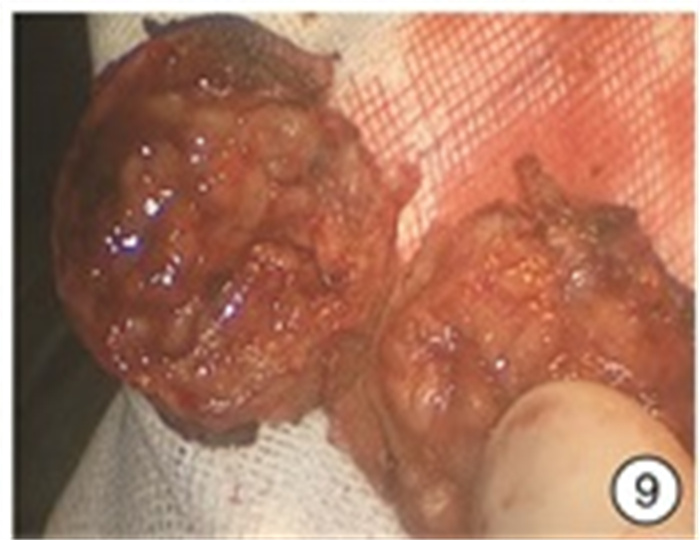
Experience of 980 nm semiconductor red laser aided "zero ischemia" retroperitoneal laparoscopic partial nephrectomy
-
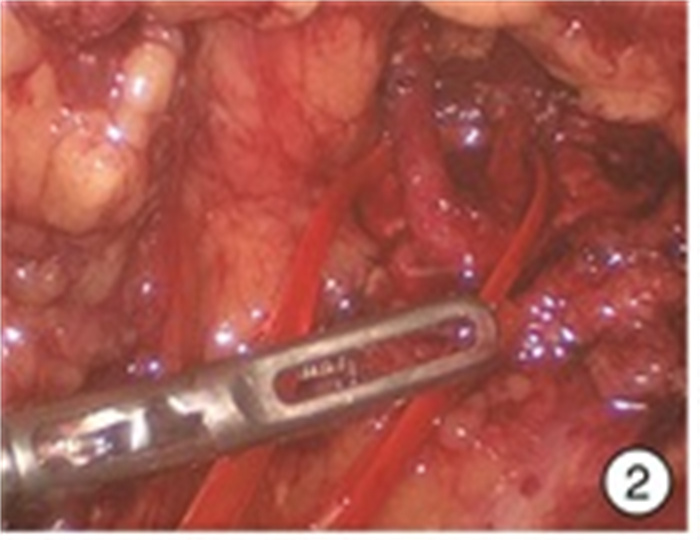
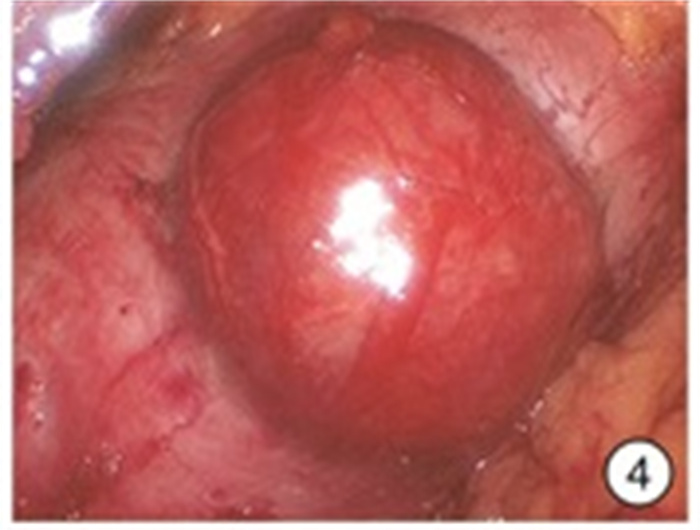
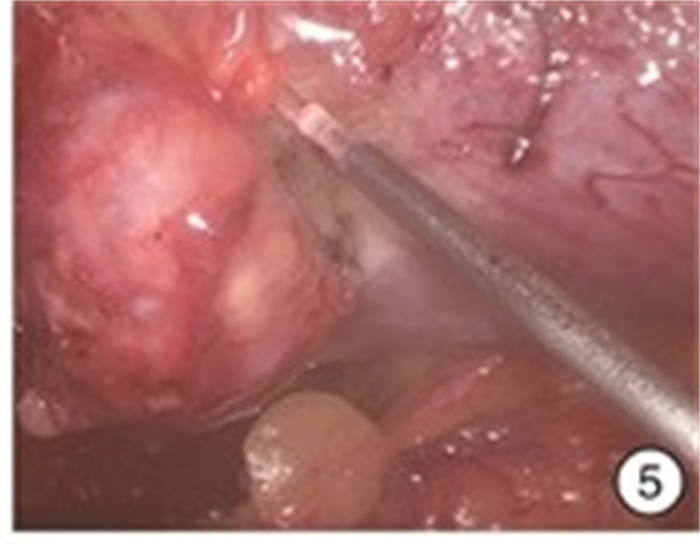
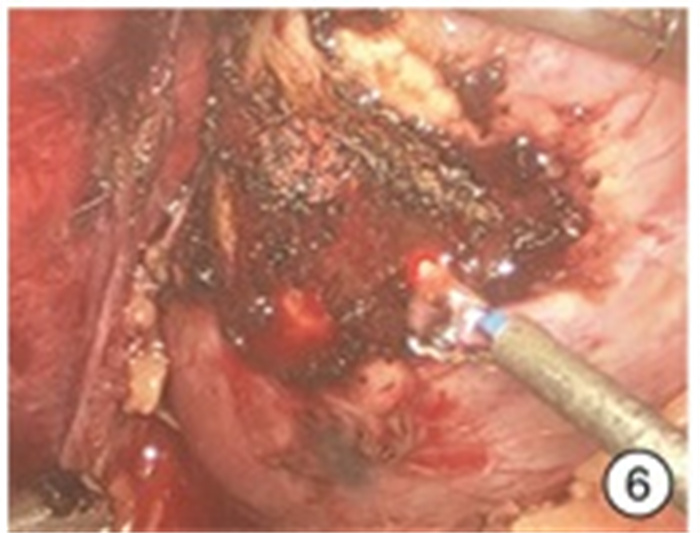
摘要: 目的 探讨980 nm半导体红激光辅助后腹腔镜下“零缺血”肾部分切除术的安全性和疗效。方法 回顾性分析2018年6月—2020年6月杭州市第一人民医院泌尿外科住院同意接受980 nm半导体红激光辅助“零缺血”后腹腔镜下肾部分切除术的外生型肾肿瘤患者的临床资料,其中男15例,女4例; 年龄38~75岁,平均(55.4±10.7)岁; 肿瘤直径2.1~4.0 cm,平均(3.22±0.75) cm; 左侧8例,右侧11例; 所有病例R.E.N.A.L.评分均为4~7分。19例患者均采用980 nm半导体红激光在不阻断肾动脉下行后腹腔镜下肾部分切除术。采用西班牙斗牛士公司红激光机、配套光纤(直径为550 μm)以及配套光纤手件。结果 19例均顺利完成手术,均未阻断肾动脉,无中转开放手术或根治性肾全切术。手术时间104~178 min,平均(133.95±20.67) min; 术中出血量50~280 mL,平均(158.42±70.65) mL; 术后拔除引流管时间4~8 d,平均(5.84±1.25) d; 术后住院天数8~17 d,平均(10.42±2.29) d。切缘均为阴性,无术后出血及其他严重并发症发生。术后3个月复查肾功能,术前平均血清肌酐(97.84±34.95) μmol/L; 术后3个月平均血清肌酐(101.68±36.32) μmol/L,差异无统计学意义(P=0.74)。术后病理结果透明细胞癌12例,血管平滑肌脂肪瘤7例。长期随访6~24个月,未见肿瘤复发或转移。结论 在后腹腔镜肾部分切除术中,应用980 nm半导体红激光行肾部分切除,无需阻断肾动脉,实现“零缺血”下切除肾肿瘤,是可行及安全的。在进一步动物实验及临床大样本研究结果支持下,该手术方式可进一步临床推广。Abstract: Objective To investigate the safety and efficacy of 980 nm semiconductor red laser aided "zero ischemia" retroperitoneal laparoscopic partial nephrectomy.Methods A retrospective analysis was performed on the clinical data of 15 males and 4 females who were admitted to the urology department of Hangzhou First People's Hospital from June 2018 to June 2020 and agreed to receive 980 nm semiconductor red laser aided "zero ischemia" retroperitoneal laparoscopic partial nephrectomy. The age was 38-75 years, with an average of (55.4±10.7) years. The tumor diameter was 2.1-4.0 cm, with an average of (3.22±0.75) cm. There were 8 cases on the left and 11 cases on the right, the R.E.N.A.L. score was 4-7 points in all the cases. All the 19 patients were treated with 980nm semiconductor red laser laparoscopic partial nephrectomy without blocking renal artery. Spanish matador red laser machine, matching optical fiber (550 μm in diameter) and matching optical fiber hand parts were used.Results All the 19 cases were completed the operation successfully, without blocking the renal artery, transferring to open surgery or radical nephrectomy. The operative time was 104-178 min, with an average of (133.95±20.67) min. Intraoperative blood loss was 50-280 mL, with an average of (158.42±70.65) mL. The removal time of drainage tube was 4-8 days after operation, with an average of (5.84±1.25) days. Postoperative hospitalization days ranged from 8 to 17 days, with an average of (10.42±2.29) days. All the surgical margins were negative, and no postoperative bleeding or other serious complications occurred. Renal function was rechecked 3 months after the operation. Preoperative mean serum creatinine was (97.84±34.95) μmol/L. The mean serum creatinine at 3 months after surgery was (101.68±36.32) μmol/L, suggesting no statistically significant difference (P=0.74). Postoperative pathology revealed 12 cases of clear cell carcinoma and 7 cases of angiomyolipoma. Long-term follow-up of 6-24 months showed no tumor recurrence or metastasis.Conclusion It is feasible and safe to perform retroperitoneal laparoscopic partial nephrectomy with 980 nm semiconductor red laser without blocking renal artery. With the support of further animal experiments and large clinical sample study results, this surgical method can be further promoted in clinical practice.
-
Key words:
- semiconductor red laser /
- zero ischemia /
- laparoscopic /
- partial nephrectomy
-

-
[1] Clark M A, Shikanov S, Raman J D, et al. Chronic kidney disease before and after partial nephrectomy[J]. J Urol, 2010, 185(1): 43-48.
[2] 徐刚, 张国玺, 邹晓峰, 等. 腹腔镜辅助小切口"零缺血"巨大肾血管平滑肌脂肪瘤切除术9例报告[J]. 临床泌尿外科杂志, 2020, 35(5): 354-357. https://www.cnki.com.cn/Article/CJFDTOTAL-LCMW202005005.htm
[3] Porpiglia F, Renard J, Billia M, et al. Is renal warm ischemia over 30 minutes during laparoscopic partial nephrecto-my possible? one year results of a prospective study[J]. EurUrol, 2007, 52(4): 1170-1178.
[4] Erol A, Cam K, Tekin A, et al. High power diode laser vaporization of the prostate: preliminary results for benign prostatic hyperplasia[J]. J Urol, 2009, 182(3): 1078-1082. doi: 10.1016/j.juro.2009.05.043
[5] Clemente Ramos LM. High power 980 nm diode laser: preliminary results in the treatment of benign prostatic hyperplasia[J]. Arch Esp Urol, 2009, 62(2): 125-130.
[6] Heuer R, Gill IS, Guazzoni G, et al. A critical analysis of the actual role of minimally invasive surgery and active surveillance for kidney cancer[J]. Eur Urol, 2010, 57(2): 223-232. doi: 10.1016/j.eururo.2009.10.023
[7] Thompson RH, Lane BR, Lohse CM, et al. Every minute counts when the renal hilum is clamped during partial nephrectomy[J]. Eur Urol, 2010, 58(3): 340-345. doi: 10.1016/j.eururo.2010.05.047
[8] Guseinov RG, Popov SV, Gorshkov AN, et al. Effects of the of renal warm ischemia time on the recovery of filtration function in the experiment[J]. Urologiia, 2017, (6): 20-29.
[9] Hou W, Ji Z. Achieving zero ischemia in minimally invasive partial nephrectomy surgery[J]. Int J Surg, 2015, 18: 48-54. doi: 10.1016/j.ijsu.2015.04.046
[10] Kyriazis I, Ozsoy M, Kallidonis P, et al. Current evidence on lasers in laparoscopy: partial nephrectomy[J]. World J Urol, 2015, 33(4): 589-594. doi: 10.1007/s00345-014-1343-0
[11] Yunanto A, Wahyudi I, Hamid A, et al. Zero ischaemia open partial nephrectomy using Thulium laser in pediatric renal tumor: A first experience[J]. Urol Case Rep, 2018, 19: 45-47. doi: 10.1016/j.eucr.2018.04.006
[12] Drerup M, Magdy A, Hager M, et al. Non-ischemic laparoscopic partial nephrectomy using 1318-nm diode laser for small exophytic renal tumors[J]. BMC Urol, 2018, 18(1): 99. doi: 10.1186/s12894-018-0405-9
[13] Khoder WY, Sroka R, Siegert S, et al. Outcome of laser-assisted laparoscopic partial nephrectomy without ischaemia for peripheral renal tumours[J]. World J Urol, 2012, 30(5): 633-638. doi: 10.1007/s00345-011-0807-8
[14] Knezevic N, Kulis T, Maric M, et al. Laparoscopic partial nephrectomy with diode laser: a promising technique[J]. Photomed Laser Surg, 2014, 32(2): 101-105. doi: 10.1089/pho.2013.3646
[15] Wang Y, Shao J, Lü Y, et al. Thulium Laser-Assisted Versus Conventional Laparoscopic Partial Nephrectomy for the Small Renal Mass[J]. Lasers Surg Med, 2020, 52(5): 402-407. doi: 10.1002/lsm.23153
[16] Lotan Y, Gettman MT, Ogan K, et al. Clinical use of the holmium: YAG laser in laparoscopic partial nephrectomy[J]. J Endourol, 2002, 16(5): 289-292. doi: 10.1089/089277902760102767
[17] 王启飞, 车翔宇, 姜涛, 等. 腹腔镜下零缺血免缝合钬激光肾部分切除术的临床应用价值[J]. 医学与哲学, 2017, 38(22): 41-44. https://www.cnki.com.cn/Article/CJFDTOTAL-YXZL201711018.htm
[18] 栾阳, 吴立成, 徐浩, 等. 铥激光在零缺血后腹腔镜肾脏小肿瘤切除术中的应用[J]. 现代泌尿生殖肿瘤杂志, 2019, 11(4): 223-226. https://www.cnki.com.cn/Article/CJFDTOTAL-PXDM201904008.htm
[19] 王伟, 王剑松, 陈戬, 等. 后腹腔镜下肾脏肿瘤铥激光部分切除术10例报告[J]. 国际泌尿系统杂志, 2017, 37(3): 345-348.
[20] 徐维锋, 纪志刚, 刘广华, 等. 后腹腔镜下双波长激光辅助零缺血肾部分切除术16例报告[J]. 临床泌尿外科杂志, 2019, 34(1): 6-8, 13. https://www.cnki.com.cn/Article/CJFDTOTAL-LCMW201901002.htm
[21] 王杭, 朱延军, 姜帅, 等. 双波长激光腹腔镜下不阻断肾动脉保留肾单位手术的疗效[J]. 中华泌尿外科杂志, 2017, 38(7): 511-514. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGJG201802135.htm
[22] Bui MH, Breda A, Gui D, et al. Less smoke and minimal tissue carbonization using a thulium laser for laparoscopic partial nephrectomy without hilar clamping in a porcine model[J]. J Endourol, 2007, 21(9): 1107-1011.
[23] Zhang Z, Zhao J, Dong W, et al. Acute Kidney Injury after Partial Nephrectomy: Role of Parenchymal Mass Reduction and Ischemia and Impact on Subsequent Functional Recovery[J]. Eur Urol, 2016, 69(4): 745-752.
[24] Mattioli S, Muñoz R, Recasens R, et al. What does Revolix laser contribute to partial nephrectomy?[J]. Arch Esp Urol, 2008, 61(9): 1126-1129.
[25] Gruschwitz T, Stein R, Schubert J, et al. Laser-supported partial nephrectomy for renal cell carcinoma[J]. Urology, 2008, 71(2): 334-336
-




 下载:
下载: