Improved methods of placing the water storage sac in the inflatable penile prothesis implantation: report of 30 cases
-
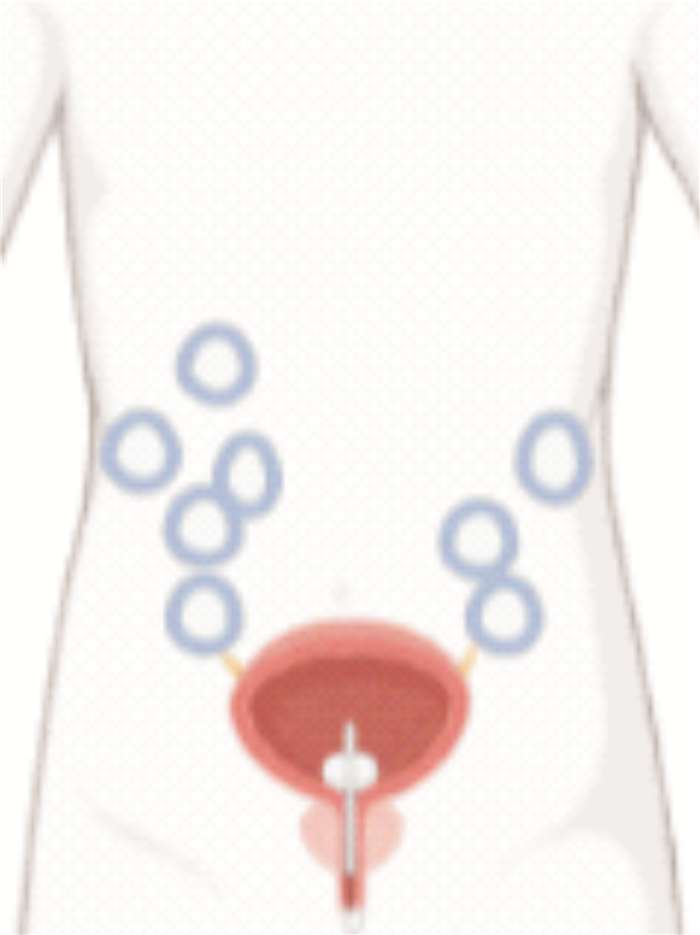
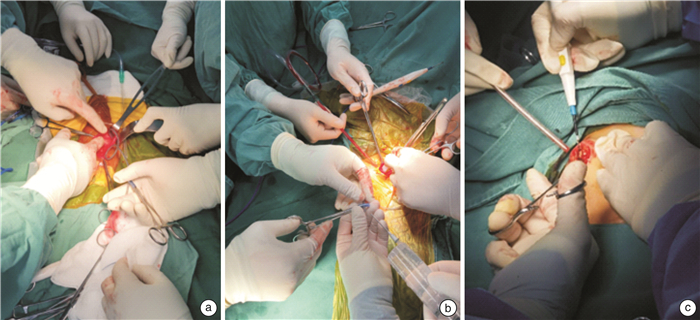
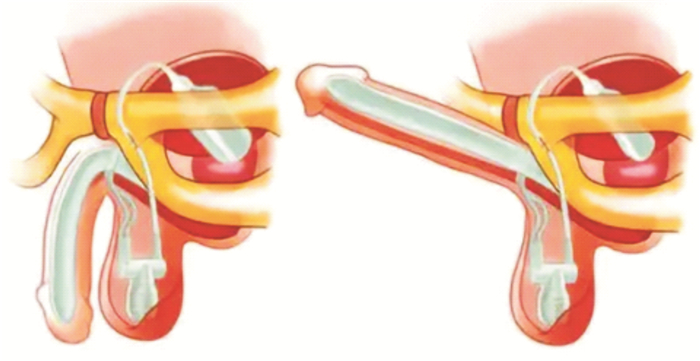
摘要: 目的 可膨胀性人工海绵体植入术常规将储水囊放置于耻骨后膀胱前间隙,而对于盆腔外伤或手术的重度勃起功能障碍患者,储水囊放置存在风险与困难。本研究旨在改良可膨胀性人工海绵体植入术的储水囊放置方法,评估其安全性与有效性。方法 回顾性分析2017年6月—2021年12月在上海市第一人民医院泌尿男科实施可膨胀性人工海绵体植入术患者的临床资料。其中对照组为常规将储水囊置于耻骨后膀胱前间隙的患者,试验组为因盆腔外伤手术实施改良储水囊植入的患者。通过门诊或电话交流对患者进行术后回访,分析改良方案的安全性、有效性。结果 30例可膨胀性人工海绵体植入术中采用改良储水囊放置的试验组患者有8例,其中放置于右侧腹壁下腹膜前间隙的有5例(16.67%),放置于左侧腹壁下腹膜前间隙的有3例(10.00%),均通过隧道法连接储水囊和泵阀。其余22例(73.33%)为对照组患者。30例手术的二次手术率为3.33%(1/30),为对照组中的1例术后泵阀故障的患者。试验组二次手术率为0(0/8),对照组为4.55%(1/22)。试验组性生活满意度为100%(8/8),对照组为90.91%(20/22)。试验组不良反应发生率为12.50%(1/8),对照组为13.64%(3/22)。结论 可膨胀性人工海绵体植入术是治疗难治性勃起功能障碍的推荐治疗方法,然而对于曾行骨盆骨折或尿道断裂相关手术的严重外伤性勃起功能障碍患者实施常规放置储水囊于耻骨后膀胱前间隙的操作存在一定风险和困难。对这类患者实施储水囊放置于左右腹壁下腹膜前间隙并通过隧道法连接储水囊与泵阀的改良方案可以简化手术操作,降低手术风险,且与常规放置方案之间在二次手术率、性生活满意度和不良反应发生率等方面没有统计学差异,显示出良好的安全性及有效性。Abstract: Objective In the inflatable penile prothesis implantation, the water storage sac is conventionally placed in the posterior space of pubic, before the bladder. For patients with severe erectile dysfunction due to pelvic trauma or surgery, there are risks and difficulties in the placement of the water storage sac. The purpose of this study is to improve the placement method of the water storage sac for the inflatable penile prothesis implantation, and to evaluate its safety and effectiveness.Methods The inflatable penile prothesis implantations performed in the Department of Andrology of Shanghai General Hospital from June 2017 to December 2021 were retrospectively analyzed. For the control group, the water storage sac was conventionally placed in the posterior space of pubic, before the bladder, while the improved water storage sac implantation was conducted for the experimental group due to pelvic trauma or surgery. Postoperative follow-up visits were carried out through outpatient clinics or telephone communication to analyze the safety and effectiveness of the improved method.Results In 30 cases of inflatable penile prothesis implantation, 8 cases (26.67%) were conducted improved methods in the experimental group. There were 5 cases (16.67%) in the preperitoneal space under the right abdominal wall, and 3 cases (10.00%) in the preperitoneal space under the left abdominal wall, in all of which the water storage sac was connected to the pump through the tunnel method. The remaining 22 cases (73.33%) were in the control group. The reoperation rate of 30 cases was 3.33% (1/30), which was 1 patient in the control group with postoperative pump failure. The reoperation rate in the experimental group was 0 (0/8), and that in the control group was 4.55% (1/22). The sexual satisfaction rate in the experimental group was 100% (8/8) and that in the control group was 90.91% (20/22). The incidence of adverse effects in the experimental group was 12.50% (1/8) and that in the control group was 13.64% (3/22).Conclusion Inflatable penile prothesis implantation is the recommended treatment for refractory erectile dysfunction. However, for patients with severe traumatic erectile dysfunction who have undergone pelvic fracture or urethral rupture related surgery, it takes certain risks and difficulties to place the water storage sac in the posterior space of pubic, before the bladder. For these patients, the improved method of placing the water storage sac in the preperitoneal space under the left or right abdominal walls and connecting the water storage sac to the pump through the tunnel method can simplify the operation and reduce the risk of surgery. There is no statistical difference in the reoperation rate, sexual satisfaction and the incidence of adverse effects between the experimental group and the other one. Thus, this improved method shows good safety and effectiveness.
-

-
[1] Medina-Polo J, García-Gómez B, Alonso-Isa M, et al. Clinical guidelines on erectile dysfunction surgery: EAU-AUA perspectives[J]. Actas Urol Esp(Engl Ed), 2020, 44(5): 289-293. doi: 10.1016/j.acuro.2019.10.008
[2] Mulcahy JJ. The Development of Modern Penile Implants[J]. Sex Med Rev, 2016, 4(2): 177-189. doi: 10.1016/j.sxmr.2015.11.003
[3] 中华医学会男科学分会, 创伤性勃起功能障碍诊疗中国专家共识编写组. 创伤性勃起功能障碍诊疗中国专家共识[J]. 中华男科学杂志, 2021, 27(6): 557-566. https://www.cnki.com.cn/Article/CJFDTOTAL-NKXB202106019.htm
[4] Chung E, Mulhall J. Practical Considerations in Inflatable Penile Implant Surgery[J]. J Sex Med, 2021, 18(8): 1320-1327. doi: 10.1016/j.jsxm.2021.05.017
[5] 陈斌, 闫立新, 马名夺, 等. 国产可膨胀性阴茎三件套假体植入术治疗29例勃起功能障碍患者的临床应用[J]. 临床泌尿外科杂志, 2016, 31(10): 918-920. https://www.cnki.com.cn/Article/CJFDTOTAL-LCMW201610016.htm
[6] 陈明, 王润, 柳靖. 阴茎假体植入术的临床应用与手术技巧(附光盘)[J]. 现代泌尿外科杂志, 2015, 20(1): 1-3. https://www.cnki.com.cn/Article/CJFDTOTAL-MNWK201501004.htm
[7] Hudak SJ. Reservoir Placement Considerations During Inflatable Penile Prosthesis Surgery[J]. Curr Urol Rep, 2019, 20(2): 8. doi: 10.1007/s11934-019-0871-y
[8] Swanton AR, Munarriz RM, Gross MS. Updates in penile prosthesis infections[J]. Asian J Androl, 2020, 22(1): 28-33. doi: 10.4103/aja.aja_84_19
[9] 方建伟, 陈慧兴, 宁晔, 等. 阴茎假体再次植入术原因分析与治疗体会(附8例报告)[J]. 中国男科学杂志, 2010, 24(10): 49-52. doi: 10.3969/j.issn.1008-0848.2010.10.013
[10] 郭庆华, 张立元, 陈小勇. 可膨胀阴茎支撑体植入术的临床治疗与随访研究[J]. 中国男科学杂志, 2014, (11): 30-32, 36. doi: 10.3969/j.issn.1008-0848.2014.11.007
[11] Segal RL, Siegelbaum MH, Lerner BD, et al. Inflatable Penile Prosthesis Implantation in the Ambulatory Setting: A Systematic Review[J]. Sex Med Rev, 2020, 8(2): 338-347. doi: 10.1016/j.sxmr.2019.07.006
[12] Frydman V, Pinar U, Abdessater M, et al. Long-term outcomes after penile prosthesis placement for the Management of Erectile Dysfunction: a single-Centre experience[J]. Basic Clin Androl, 2021, 31(1): 4. doi: 10.1186/s12610-021-00123-x
[13] Nguyen HMT, Gabrielson AT, Hellstrom WJG. Erectile Dysfunction in Young Men-A Review of the Prevalence and Risk Factors[J]. Sex Med Rev, 2017, 5(4): 508-520. doi: 10.1016/j.sxmr.2017.05.004
[14] Scherzer ND, Dick B, Gabrielson AT, et al. Penile Prosthesis Complications: Planning, Prevention, and Decision Making[J]. Sex Med Rev, 2019, 7(2): 349-359. doi: 10.1016/j.sxmr.2018.04.002
[15] Zaazaa A, Mostafa T. Spontaneous Penile Tumescence by Sparing Cavernous Tissue in the Course of Malleable Penile Prosthesis Implantation[J]. J Sex Med, 2019, 16(3): 474-478. doi: 10.1016/j.jsxm.2019.01.012
[16] Levine LA, Becher EF, Bella AJ, et al. Penile Prosthesis Surgery: Current Recommendations From the International Consultation on Sexual Medicine[J]. J Sex Med, 2016, 13(4): 489-518. doi: 10.1016/j.jsxm.2016.01.017
[17] 张修举, 王福, 郭军. 2018年AUA勃起功能障碍指南解读[J]. 中国男科学杂志, 2019, 33(2): 75-76. https://www.cnki.com.cn/Article/CJFDTOTAL-NXXX201902018.htm
[18] Madiraju SK, Hakky TS, Perito PE, et al. Placement of Inflatable Penile Implants in Patients With Prior Radical Pelvic Surgery: A Literature Review[J]. Sex Med Rev, 2019, 7(1): 189-197. doi: 10.1016/j.sxmr.2018.10.002
[19] 刘天琦, 方建雄, 刘豪圣, 等. 干细胞治疗前列腺癌根治术后勃起功能障碍的临床研究进展[J]. 临床泌尿外科杂志, 2020, 35(11): 924-928. https://www.cnki.com.cn/Article/CJFDTOTAL-LCMW202011017.htm
[20] Narang GL, Figler BD, Coward RM. Preoperative counseling and expectation management for inflatable penile prosthesis implantation[J]. Transl Androl Urol, 2017, 6(Suppl 5): S869-S880.
[21] Bettocchi C, Osmonov D, van Renterghem K, et al. Management of Disastrous Complications of Penile Implant Surgery[J]. J Sex Med, 2021, 18(7): 1145-1157. doi: 10.1016/j.jsxm.2021.04.003
-




 下载:
下载: