-
摘要: 十二指肠损伤属于腹腔镜肾切除术的少见并发症,具有损伤隐匿、后果严重、治疗棘手的特点,如发现不及时或者处置不当极易导致患者死亡。回顾性分析我院2例腹腔镜肾切除术伴十二指肠损伤患者的诊断方法和治疗措施,得出以下经验体会:腹腔镜肾切除术并发十二指肠损伤改善患者预后的关键在于早期诊断,重点在于手术干预为主、留置空肠引流管,辅助术后抗感染、充分引流及营养支持的综合治疗。Abstract: Duodenal injury is a rare complication of laparoscopic nephrectomy, which has the characteristics of hidden injury, serious consequences and difficult treatment. If it is not found in time or handled improperly, it is very easy to lead to the death of patients. The diagnostic methods and treatment measures of 2 patients with duodenal injury after laparoscopic nephrectomy in our hospital were retrospectively analyzed. The following experience was obtained: the key to the prognosis of patients with duodenal injury after laparoscopic nephrectomy is early diagnosis. The important points are comprehensive treatments including surgical intervention, jejunal drainage tube indwelling, postoperative anti-infection, sufficient drainage and adequate nutritional support.
-
Key words:
- laparoscope /
- nephrectomy /
- duodenal injury /
- complication
-

-
[1] 赵健, 符伟军, 洪宝发, 等. 经腹腔机器人精准肾根治性切除术手术要点及应用体会[J]. 微创泌尿外科杂志, 2017, 6(5): 257-260. https://www.cnki.com.cn/Article/CJFDTOTAL-WCMN201705002.htm
[2] Choi K, Hill S, Hale N, et al. Intraoperative mannitol during robotic-assisted-laparoscopic partial nephrectomy[J]. J Robot Surg, 2019, 13(3): 401-405. doi: 10.1007/s11701-018-0868-4
[3] Machado NO. Duodenal injury post laparoscopic cholecystectomy: incidence, mechanism, management and outcome[J]. World J Gastrointest Surg, 2016, 8(4): 335-344. doi: 10.4240/wjgs.v8.i4.335
[4] Bishoff JT, Allaf ME, Kirkels W, et al. Laparoscopic bowel injury: incidence and clinical presentation[J]. J Urol, 1999, 161(3): 887-890. doi: 10.1016/S0022-5347(01)61797-X
[5] Pareek G, Hedican SP, Gee JR, et al. Meta-analysis of the complications of laparoscopic renal surgery: comparison of procedures and techniques[J]. J Urol, 2006, 175(4): 1208-1213. doi: 10.1016/S0022-5347(05)00639-7
[6] Shigemura K, Yasufuku T, Arakawa S, et al. Efficacy of early use of snake retractor in retroperitoneoscopic nephrectomy or nephroureterectomy[J]. J Endourol, 2010, 24(11): 1771-1774. doi: 10.1089/end.2009.0550
[7] Upadhyaya M, Sundararajan LS, Woodward MN. Dangerous deliveries: lessons learned during retroperitoneal specimen retrieval[J]. J Pediatr Surg, 2011, 46(4): e13-e15. doi: 10.1016/j.jpedsurg.2010.10.031
[8] Ramasamy R, Afaneh C, Katz M, et al. Comparison of complications of laparoscopic versus laparoendoscopic single site donor nephrectomy using the modified Clavien grading system[J]. J Urol, 2011, 186(4): 1386-1390. doi: 10.1016/j.juro.2011.05.053
[9] Joshi SS, Sundaram CP. Small bowel injury during laparoendoscopic single-site surgery for simple nephrectomy[J]. JSLS, 2013, 17(1): 167-169. doi: 10.4293/108680812X13517013317112
[10] 杨锦建, 顾朝辉, 丁映辉. 泌尿外科腹腔镜手术并发症的处理策略[J]. 临床泌尿外科杂志, 2017, 32(2): 83-87. https://www.cnki.com.cn/Article/CJFDTOTAL-LCMW201702001.htm
[11] Overbey DM, Townsend NT, Chapman BC, et al. Surgical energy-based device injuries and fatalities reported to the Food and Drug Administration[J]. J Am Coll Surg, 2015, 221(1): 197-205.e1. doi: 10.1016/j.jamcollsurg.2015.03.031
[12] Avrutis O, Meshoulam J, Yutkin O, et al. Brief clinical report: duodenal laceration presenting as massive hematemesis and multiple intraabdominal abscesses after laparoscopic cholecystectomy[J]. Surg Laparosc Endosc Percutan Tech, 2001, 11(5): 330-333. doi: 10.1097/00129689-200110000-00009
[13] Ansari D, Torén W, Lindberg S, et al. Diagnosis and management of duodenal perforations: a narrative review[J]. Scand J Gastroenterol, 2019, 54(8): 939-944. doi: 10.1080/00365521.2019.1647456
[14] Popović M, Colović R, Milićević M, et al. Surgical treatment of peroperative injuries of the duodenum[J]. Acta Chir Iugosl, 1994, 41(1): 49-51.
-

| 引用本文: | 赵健, 符伟军, 宋勇, 等. 腹腔镜肾切除术并发十二指肠损伤2例[J]. 临床泌尿外科杂志, 2022, 37(5): 406-408. doi: 10.13201/j.issn.1001-1420.2022.05.015 |
| Citation: | ZHAO Jian, FU Weijun, SONG Yong, et al. Two cases of duodenal injury after laparoscopic nephrectomy[J]. J Clin Urol, 2022, 37(5): 406-408. doi: 10.13201/j.issn.1001-1420.2022.05.015 |
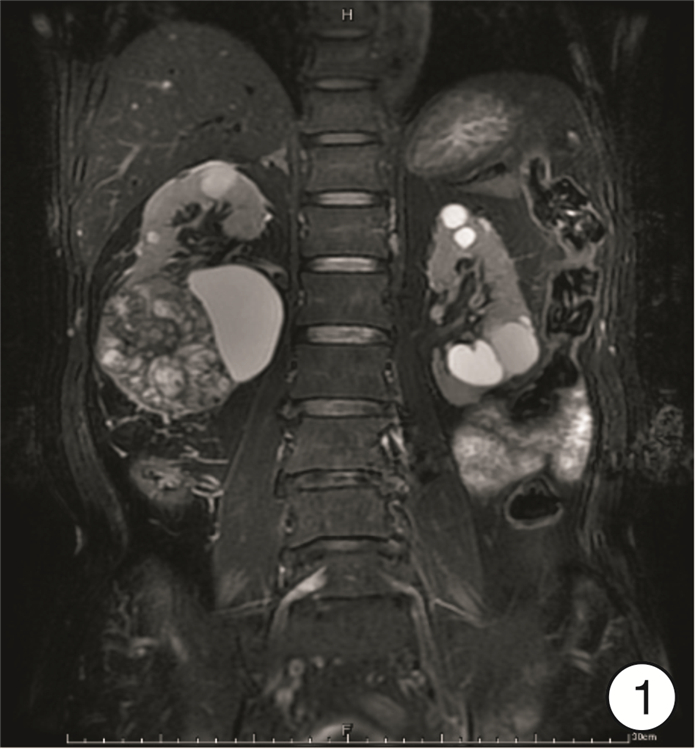
- Figure 1.
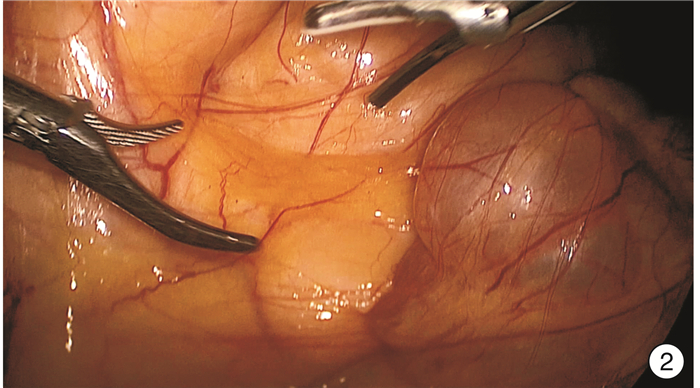
- Figure 2.
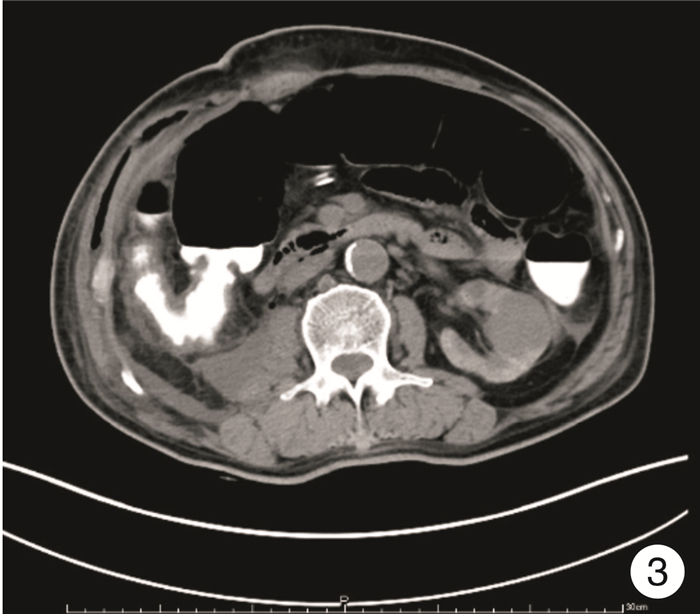
- Figure 3.



 下载:
下载: