-
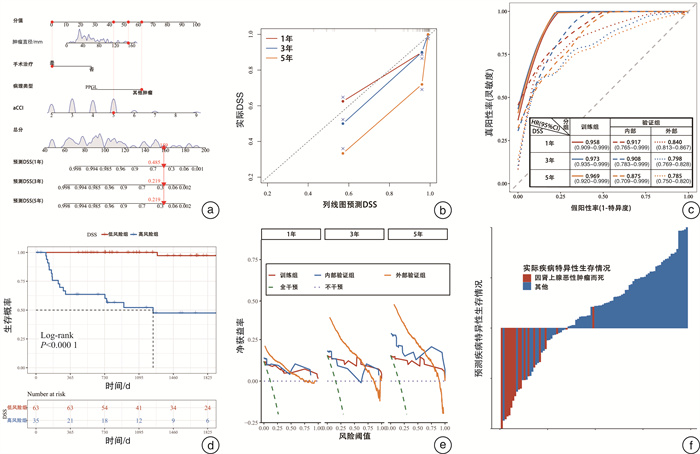
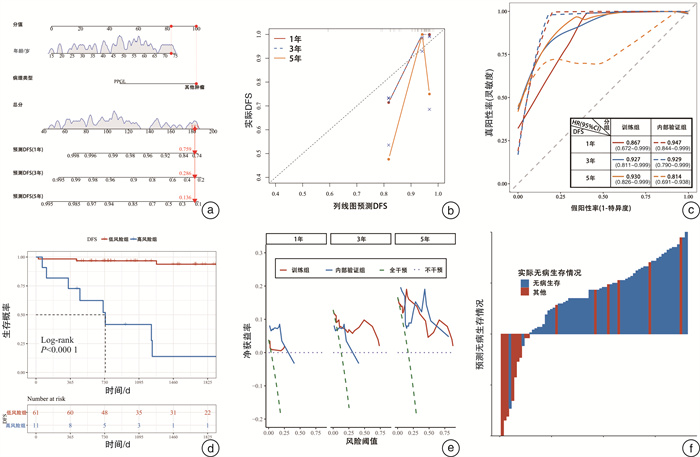
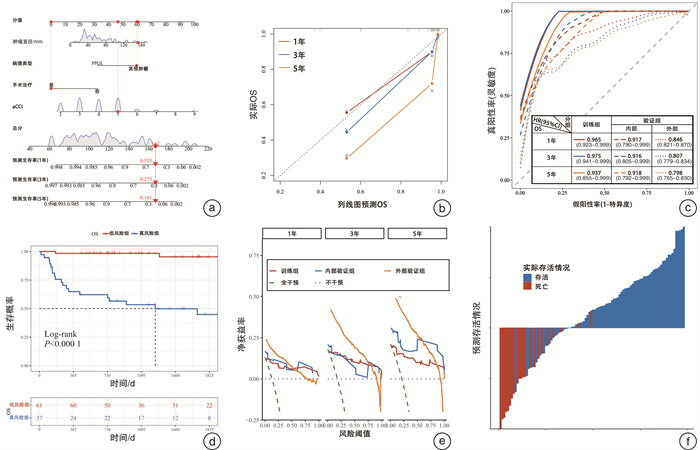
摘要: 目的 分析肾上腺恶性肿瘤患者的生存情况,构建模型并进行验证。方法 回顾性收集2014年8月—2021年12月就诊于山西白求恩医院的肾上腺恶性肿瘤患者,将患者按照7∶3的比例随机分为训练组和内部验证组。训练组用来模型构建,内部验证组用于验证模型准确度。另选取SEER数据库中肾上腺恶性肿瘤患者进行外部验证。通过单因素Cox回归与多因素Cox回归筛选独立影响因素,构建列线图,采用受试者工作特征(receiver operating characteristic,ROC)曲线分析列线图的预测效能,采用C指数和Bootstrap自抽样法验证列线图的区分度和一致性。结果 影响总生存期(overall survival,OS)的独立影响因素包括:年龄校正卡尔森合并症指数(age-adjusted charlson comorbidity index,aCCI)、肿瘤直径、病理类型、手术治疗。疾病特异生存期(disease-specific survival,DSS)的独立影响因素包括:aCCI、肿瘤直径、病理类型、手术治疗。术后患者无病生存期(disease-free survival,DFS)的独立影响因素包括:年龄和病理类型。根据筛选结果构建模型,三者的C指数分别为0.944、0.944、0.857,临床决策曲线提示其分别可提高15%、13%、13%患者净获益率,说明模型预测效果良好。结论 本研究模型预测肾上腺恶性肿瘤患者1年、3年、5年的OS、DSS、DFS,有助于预估肾上腺恶性肿瘤患者的生存情况,作为肾上腺恶性肿瘤评估预后工具,便于医师针对不同患者给予个性化治疗干预,提供患者最大化收益。Abstract: Objective To analyze the survival of patients with adrenal malignant tumors, construct the model and validate it.Methods Patients with adrenal malignant tumors who visited Shanxi Bethune Hospital from August 2014 to December 2021 were retrospectively collected. The patients were randomly divided into training group and internal validation group according to the ratio of 7∶3. The training group was used to build the model, and the internal validation group was used to verify the accuracy of the model. In addition, patients with adrenal malignant tumors in SEER database were selected for external verification. The independent influence factors were screened by univariate Cox regression and multivariate Cox regression, and the prediction efficiency of the nomogram was analyzed by ROC curve, and the C-index and Bootstrap self-sampling methods were used to verify the discrimination and consistency of the nomogram.Results Independent influence factors affecting overall survival(OS) included age-adjusted Charlson comorbidity index(aCCI), tumor diameter, pathological type, and surgical treatment. Independent factors influencing disease-specific survival(DSS) included aCCI, tumor diameter, pathology type, and surgical treatment. Independent factors influencing postoperative disease-free survival(DFS) included age and pathological type. According to the screening results, the C indices of the three were 0.944, 0.944 and 0.857, and the clinical decision curves showed that they could increase the net benefit rate of patients by 15%, 13% and 13%, respectively, indicating that the model had a good prediction effect.Conclusion This research model predicts the OS, DSS and DFS of patients with adrenal malignant tumors for 1, 3 and 5 years, and is helpful to predict the survival of patients with adrenal malignant tumors. As a prognosis tool for assessing the survival of patients with adrenal malignant tumors, it is convenient for physicians to give personalized treatment interventions for different patients and provide patients with maximum benefits.
-
Key words:
- adrenal glands /
- malignant tumor /
- prediction models /
- nomogram /
- survival
-

-
表 1 患者基线资料
例(%),X±S,M(P25,P75) 变量 总队列(98例) 分组 t/Z/χ2 P值 训练组(69例) 内部验证组(29例) 基本病例数据 年龄/岁 52.50(40.25,62.50) 52.00(40.00,61.00) 53.00(43.00,65.00) 0.662 0.511 性别 0.284 0.594 男 50(51.0) 34(49.3) 16(55.2) 女 48(49.0) 35(50.7) 13(44.8) BMI/(kg/m2) 23.21(20.97,24.61) 23.44(21.01,25.16) 22.79(20.70,24.09) 1.140 0.256 高血压史 1.342 0.247 无 46(46.9) 35(50.7) 11(37.9) 有 52(53.1) 34(49.3) 18(62.1) 糖尿病史 0.148 0.700 无 80(81.6) 57(82.6) 23(79.3) 有 18(18.4) 12(17.4) 6(20.7) 冠心病史 0.737 0.391 无 84(85.7) 61(88.4) 23(79.3) 有 14(14.3) 8(11.6) 6(20.7) 脑梗史 0.001 0.999 无 88(89.8) 62(89.9) 26(89.7) 有 10(10.2) 7(10.1) 3(10.3) 吸烟史 0.481 0.488 无 66(67.3) 45(65.2) 21(72.4) 有 32(32.7) 24(34.8) 8(27.6) 肿瘤史 1.325 0.250 无 81(82.7) 59(85.5) 22(75.9) 有 17(17.3) 10(14.5) 7(24.1) 肿瘤史 0.025 0.873 无 62(63.3) 44(63.8) 18(62.1) 有 36(36.7) 25(36.2) 11(37.9) 输血史 0.073 0.787 无 76(77.6) 53(76.8) 23(79.3) 有 22(22.4) 16(23.2) 6(20.7) aCCI 4.00(3.00,5.00) 4.00(3.00,5.00) 4.00(3.00,5.00) 1.253 0.201 血红蛋白/(g/L) 130.45±19.13 130.85±18.32 129.49±21.26 0.318 0.751 肿瘤情况 病理类型 2.538 0.468 PPGL 62(63.3) 45(65.2) 17(58.6) ACC 19(19.4) 14(20.3) 5(17.2) 肾上腺转移癌 12(12.2) 8(11.6) 4(13.8) 其他 5(5.1) 2(2.9) 3(10.3) 肿瘤分侧 0.580 0.748 左侧 35(35.7) 25(36.2) 10(34.5) 右侧 53(54.1) 38(55.1) 15(51.7) 双侧 10(10.2) 6(8.7) 4(13.8) 肿瘤直径/mm 53.00(35.00,77.75) 53.00(35.00,78.00) 53.00(36.00,77.00) 0.027 0.981 T分期 1.435 0.488 1 45(45.9) 32(46.4) 13(44.8) 2 45(45.9) 30(43.5) 15(51.7) 3 8(8.2) 7(10.1) 1(3.4) M分期 0.001 0.999 0 97(99.0) 68(98.6) 29(100.0) 1 1(1.0) 1(1.4) 0(0) AJCC分期 1.913 0.384 Ⅰ 45(45.9) 32(46.4) 13(44.8) Ⅱ 44(44.9) 29(42.0) 15(51.7) Ⅲ/Ⅳ 9(9.2) 8(11.6) 1(3.4) 治疗情况 手术治疗 0.024 0.878 无 26(26.5) 18(26.1) 8(27.6) 有 72(73.5) 51(73.9) 21(72.4) 生存情况 OS/d NR(2 826,NR) NR(2 826,NR) NR(NR,NR) 0.275 0.600 DSS/d NR(NR,NR) NR(NR,NR) NR(NR,NR) 1.031 0.310 DFS/d NR(2 460,NR) NR(2 460,NR) NR(2 250,NR) 0.010 0.920 注:NR:未达到。 -
[1] Jing Y, Hu J, Luo R, et al. Prevalence and Characteristics of Adrenal Tumors in an Unselected Screening Population: A Cross-Sectional Study[J]. Ann Intern Med, 2022, 175(10): 1383-1391. doi: 10.7326/M22-1619
[2] Karaosmanoglu AD, Onder O, Leblebici CB, et al. Cross-sectional imaging features of unusual adrenal lesions: a radiopathological correlation[J]. Abdom Radiol, 2021, 46(8): 3974-3994. doi: 10.1007/s00261-021-03041-8
[3] 李芳, 王进京, 邓会岩, 等. WHO(2017)肾上腺内分泌肿瘤新分类解读[J]. 临床与实验病理学杂志, 2018, 34(7): 709-713. doi: 10.13315/j.cnki.cjcep.2018.07.001
[4] Shah MH, Goldner WS, Benson AB, et al. Neuroendocrine and Adrenal Tumors, Version 2.2021, NCCN Clinical Practice Guidelines in Oncology[J]. J Natl Compr Canc Netw, 2021, 19(7): 839-868. doi: 10.6004/jnccn.2021.0032
[5] Mei L, Khurana A, Al-Juhaishi T, et al. Prognostic Factors of Malignant Pheochromocytoma and Paraganglioma: A Combined SEER and TCGA Databases Review[J]. Horm Metab Res, 2019, 51(7): 451-457. doi: 10.1055/a-0851-3275
[6] Zheng L, Gu Y, Silang J, et al. Prognostic Nomograms for Predicting Overall Survival and Cancer-Specific Survival of Patients With Malignant Pheochromocytoma and Paraganglioma[J]. Front Endocrinol(Lausanne), 2021, 12: 684668. doi: 10.3389/fendo.2021.684668
[7] 杜学谦, 孙青风, 田龙江. LncRNA HOTAIR、VEGF在肾上腺恶性肿瘤组织中的表达及其预后相关性[J]. 临床肾脏病杂志, 2021, 21(2): 130-135. https://www.cnki.com.cn/Article/CJFDTOTAL-LCSB202102009.htm
[8] Hescot S, Curras-Freixes M, Deutschbein T, et al. Prognosis of Malignant Pheochromocytoma and Paraganglioma(MAPP-Prono Study): A European Network for the Study of Adrenal Tumors Retrospective Study[J]. J Clin Endocrinol Metab, 2019, 104(6): 2367-2374. doi: 10.1210/jc.2018-01968
[9] Kimura N, Takayanagi R, Takizawa N, et al. Pathological grading for predicting metastasis in phaeochromocytoma and paraganglioma[J]. Endocr Relat Cancer, 2014, 21(3): 405-414. doi: 10.1530/ERC-13-0494
[10] Charlson M, Szatrowski TP, Peterson J, et al. Validation of a combined comorbidity index[J]. J Clin Epidemiol, 1994, 47(11): 1245-1251. doi: 10.1016/0895-4356(94)90129-5
[11] Takada Y, Kawashima H, Ohno E, et al. The impact of the age-adjusted Charlson comorbidity index as a prognostic factor for endoscopic papillectomy in ampullary tumors[J]. J Gastroenterol, 2022, 57(3): 199-207. doi: 10.1007/s00535-022-01853-z
[12] Di Donato V, D Oria O, Giannini A, et al. Age-Adjusted Charlson Comorbidity Index Predicts Survival in Endometrial Cancer Patients[J]. Gynecol Obstet Invest, 2022, 87(3-4): 191-199. doi: 10.1159/000525405
[13] Kang HW, Kim SM, Kim WT, et al. The age-adjusted Charlson comorbidity index as a predictor of overall survival of surgically treated non-metastatic clear cell renal cell carcinoma[J]. J Cancer Res Clin Oncol, 2020, 146(1): 187-196. doi: 10.1007/s00432-019-03042-7
[14] Ahmed AA. Adrenocortical neoplasms in young children: age as a prognostic factor[J]. Ann Clin Lab Sci, 2009, 39(3): 277-282.
[15] Wang W, Chang G, Sun Y, et al. Nomograms for Individualized Evaluation of Prognosis in Adrenocortical Carcinomas for the Elderly: A Population-Based Analysis[J]. J Invest Surg, 2022, 35(5): 1153-1160. doi: 10.1080/08941939.2021.1968981
[16] Sun S, Wang J, Yang B, et al. A nomogram for evaluation and analysis of difficulty in retroperitoneal laparoscopic adrenalectomy: A single-center study with prospective validation using LASSO-logistic regression[J]. Front Endocrinol, 2022, 13: 1004112. doi: 10.3389/fendo.2022.1004112
[17] Alberici L, Paganini AM, Ricci C, et al. Development and validation of a preoperative"difficulty score"for laparoscopic transabdominal adrenalectomy: a multicenter retrospective study[J]. Surg Endosc, 2022, 36(5): 3549-3557. doi: 10.1007/s00464-021-08678-6
[18] Pantalone KM, Gopan T, Remer EM, et al. Change in Adrenal Mass Size as a Predictor of a Malignant Tumor[J]. Endocrine Practice, 2010, 16(4): 577-587. doi: 10.4158/EP09351.OR
[19] Tan L, Ye Y, Xiao K, et al. A clinicopathological analysis of adrenal tumors in patients with history of extra-adrenal cancers[J]. BMC Cancer, 2019, 19(1): 838. doi: 10.1186/s12885-019-6061-y
[20] Minguez OC, Gomez DSV, Alvaro LJ, et al. Tumour size in adrenal tumours: its importance in the indication of adrenalectomy and in surgical outcomes-a single-centre experience[J]. J Endocrinol Invest, 2022, 45(10): 1999-2006. doi: 10.1007/s40618-022-01836-0
[21] Zahir ST, Aalipour E, Barand P, et al. Clinicopathological Features of Adrenal Tumors: a Ten-year Study in Yazd, Iran[J]. Asian Pac J Cancer Prev, 2015, 16(12): 5031-5036. doi: 10.7314/APJCP.2015.16.12.5031
[22] Shetty I, Fuller S, Raygada M, et al. Adrenocortical carcinoma masquerading as pheochromocytoma: a histopathologic dilemma[J]. Endocrinol Diabetes Metab Case Rep, 2020, 2020: 19-0147.
[23] Crona J, Beuschlein F, Pacak K, et al. Advances in adrenal tumors 2018[J]. Endocr Relat Cancer, 2018, 25(7): R405-R420. doi: 10.1530/ERC-18-0138
[24] Fassnacht M, Terzolo M, Allolio B, et al. Combination chemotherapy in advanced adrenocortical carcinoma[J]. N Engl J Med, 2012, 366(23): 2189-2197. doi: 10.1056/NEJMoa1200966
[25] Toke J, Uhlyarik A, Lohinszky J, et al. Prognostic factors and mitotane treatment of adrenocortical cancer. Two decades of experience from an institutional case series[J]. Front Endocrinol(Lausanne), 2022, 13: 952418. doi: 10.3389/fendo.2022.952418
[26] Terzolo M, Baudin AE, Ardito A, et al. Mitotane levels predict the outcome of patients with adrenocortical carcinoma treated adjuvantly following radical resection[J]. Eur J Endocrinol, 2013, 169(3): 263-270. doi: 10.1530/EJE-13-0242
[27] Habra MA, Ejaz S, Feng L, et al. A retrospective cohort analysis of the efficacy of adjuvant radiotherapy after primary surgical resection in patients with adrenocortical carcinoma[J]. J Clin Endocrinol Metab, 2013, 98(1): 192-197. doi: 10.1210/jc.2012-2367
[28] Wu K, Liu X, Liu Z, et al. Benefit of Postoperative Radiotherapy for Patients With Nonmetastatic Adrenocortical Carcinoma: A Population-Based Analysis[J]. J Natl Compr Canc Netw, 2021, 19(12): 1425-1432. doi: 10.6004/jnccn.2021.7035
[29] Gaujoux S, Bertherat J, Dousset B, et al. Laparoscopic adrenalectomy for adrenocortical carcinoma: a medico-surgical perspective[J]. Ann Endocrinol(Paris), 2012, 73(5): 441-447. doi: 10.1016/j.ando.2012.07.001
[30] Sun S, Wang Y, Yao W, et al. Development and validation of nomograms to predict survival of primary adrenal lymphoma: a population-based retrospective study[J]. Sci Rep, 2023, 13(1): 14428. doi: 10.1038/s41598-023-41839-2
-

| 引用本文: | 姚伟, 孙世伟, 王越, 等. 肾上腺恶性肿瘤预测生存列线图的建立[J]. 临床泌尿外科杂志, 2023, 38(11): 827-834. doi: 10.13201/j.issn.1001-1420.2023.11.005 |
| Citation: | YAO Wei, SUN Shiwei, WANG Yue, et al. Model to predict the survival of patients with adrenal malignant tumor[J]. J Clin Urol, 2023, 38(11): 827-834. doi: 10.13201/j.issn.1001-1420.2023.11.005 |
- Figure 1.
- Figure 2.
- Figure 3.



 下载:
下载: