ABO-incompatible living donor kidney transplantation: clinical analysis of 23 cases
-
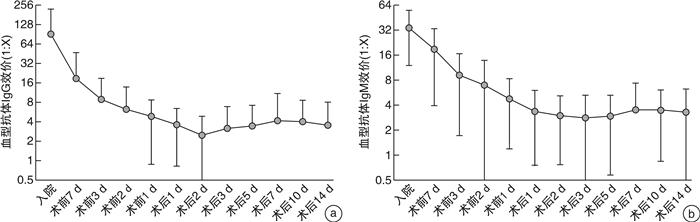
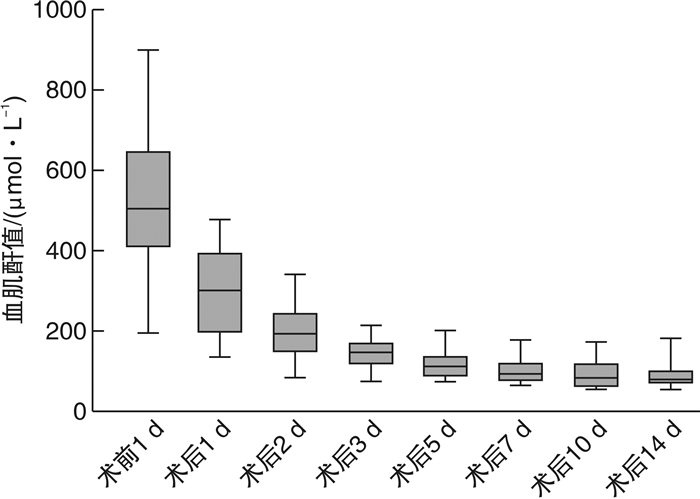
摘要: 目的 探讨ABO血型不相容肾移植(ABO incompatible kidney transplantation,ABOi-KT)临床疗效并进行相关文献复习。方法 本研究对郑州大学第一附属医院2017年5月—2021年12月施行的23例ABOi-KT供、受者的临床资料进行了回顾性分析。在23例ABOi-KT中,5例为B型供A型,6例为B型供O型,5例为AB型供A型,2例为AB型供B型,3例为A型供O型,2例为A型供B型。23例受者初始IgG血型抗体效价中,1例为1∶512,4例为1∶256,3例为1∶128,3例为1∶64,4例为1∶16,1例为1∶4,3例为1∶2,4例为阴性;23例受者初始IgM血型抗体效价中,6例为1∶64,6例为1∶32,9例为1∶16,1例为1∶8,1例为1∶4。23例受者术前均通过个体化脱敏治疗方案,并术后监测受者血型抗体效价水平变化、尿量及血肌酐值等相关指标。观察ABOi-KT受者肾功能恢复情况。结果 采用小剂量的利妥昔单抗清除B细胞[100 mg(< 50 kg)、200 mg(50~65 kg),300 mg(>65 kg)],多次血浆置换降低血型抗体滴度、免疫抑制剂提前应用抑制血型抗体反弹的个体化脱敏治疗。肾移植手术当日,23例受者血型抗体IgM、IgG效价水平均≤1∶8,其中21例受者2周内未出现血型抗体效价的反弹,围手术期无凝血功能障碍(出血倾向和血栓形成)及移植肾功能延迟恢复。1例受者于术后第3天血型抗体效价出现反弹,发生急性抗体介导排斥反应,经血浆置换等综合治疗效果差,行移植肾切除术并同期进行血型相容的二次移植,随访至今肾功能恢复正常。1例受者术后出现早期无尿,多次复查血型抗体滴度维持在(IgM 1∶16,IgG 1∶16)以下,移植肾穿刺考虑IgA肾病复发,给予6次AB型血浆置换后肾功能恢复至正常。结论 采用有效的个体化脱敏方案,ABOi-KT是安全可行的,可以一定程度上缓解供肾短缺。Abstract: Objective To explore the clinical effect of ABO incompatible kidney transplantation (ABOi-KT) and review the related literature.Methods This study conducted a retrospective analysis of the clinical data of 23 ABOi-KT donors and recipients implemented in our center from May 2017 to December 2021. Among the 23 cases of ABOi-KT, there were 5 cases of B to A, 6 cases of B to O, 5 cases of AB to A, 2 cases of AB to B, 3 cases of A to O, 2 cases of A to B. Among the initial IgG antibody titers of 23 recipients, 1 was 1∶512, 4 were 1∶256, 3 were 1∶128, 3 were 1∶64, 4 were 1∶16, 1 was 1∶4, 3 were 1∶2, 4 were negative. Among the initial IgM antibody titers of 23 recipients, 6 were 1∶64, 6 were 1∶32, 9 were 1∶16, 1 was 1∶8, and 1 was 1∶4.These 23 patients were all treated with individualized desensitization therapy before operation, and the changes of serum antibody titer, urine volume and serum creatinine were monitored after operation. The recovery of ABOi-KT receptor renal function was observed.Rusults Individualized desensitization therapy was applied including low-dose rituximab to clear B cells [100 mg (< 50 kg), 200 mg (50-65 kg), 300 mg (> 65 kg)], multiple plasma exchanges to reduce blood group antibody titers, and early application of immunosuppressants to inhibit blood group antibody rebound. The blood group antibody IgM and IgG titer levels of 23 recipients were ≤1∶8 on the day of transplantation. Among them, 21 recipients showed no rebound of blood group antibody titer within 2 weeks, and there was no coagulation dysfunction during the perioperative period (bleeding tendency and thrombosis) or delayed recovery of renal function. One recipient's blood group antibody titer rebounded on the third day after the operation, and acute antibody-mediated rejection occurred. The comprehensive treatment effect such as plasma exchange was poor, so the transplant nephrectomy was performed concurrently with a blood group compatible secondary transplantation. Renal function has returned to normal since follow-up. One patient had no urine in the early stage after operation, and the blood type antibody titer was maintained below (IgM 1∶16, IgG 1∶16) after multiple reviews. The graft kidney puncture showed the recurrence of IgA nephropathy, and the renal function recovered to normal after six times of AB type plasma exchange.Conclusion With effective individualized desensitization programs, ABOi-KT is safe and feasible and can alleviate the shortage of donor kidneys to a certain extent.
-
Key words:
- kidney transplantation /
- ABO blood type /
- antibody titer /
- desensitization treatment /
- incompatible /
- living donor
-

-
表 1 23例ABO血型不相容亲属活体肾移植的供、受者资料
病例 供体 受体 供受体关系 HLA错配数 透析 性别 年龄/岁 血型 性别 年龄/岁 血型 原发病 方式 时长/月 例1 女 54 A 男 31 O 慢性肾小球肾炎 母子 3 血液透析 12 例2 女 53 AB 男 33 A 慢性肾小球肾炎 母子 3 血液透析 36 例3 男 53 B 男 32 A 慢性肾小球肾炎 父子 3 血液透析 1 例4 女 58 B 男 30 A 慢性肾小球肾炎 母子 3 血液透析 6 例5 男 56 AB 男 32 A 慢性肾小球肾炎 父子 3 血液透析 4 例6 女 56 A 男 33 B 慢性肾小球肾炎 母子 3 血液透析 38 例7 女 58 B 男 33 O 慢性肾小球肾炎 母子 3 血液透析 5 例8 女 59 B 男 36 A 慢性肾小球肾炎 母子 3 血液透析 2 例9 女 60 A 男 33 O 慢性肾小球肾炎 母子 3 血液透析 4 例10 女 52 B 女 32 O 慢性肾小球肾炎 母女 3 血液透析 10 例11 女 62 A 女 38 B 慢性肾小球肾炎 母女 3 血液透析 3 例12 女 63 B 女 35 A 慢性肾小球肾炎 母女 3 血液透析 4 例13 女 60 AB 男 34 B 慢性肾小球肾炎 母子 3 血液透析 6 例14 女 54 AB 男 27 B 慢性肾小球肾炎 母子 3 血液透析 2 例15 女 65 A 男 37 O 慢性肾小球肾炎 母子 3 血液透析 1 例16 男 51 B 女 31 O 慢性肾小球肾炎 父女 3 血液透析 15 例17 男 60 B 男 18 A 慢性肾小球肾炎 父子 3 血液透析 6 例18 女 63 AB 女 38 A 慢性肾小球肾炎 母女 3 血液透析 4 例19 女 44 AB 男 23 A 慢性肾小球肾炎 母子 3 血液透析 11 例20 女 46 B 男 20 O 慢性肾小球肾炎 母子 3 血液透析 5 例21 女 53 B 男 30 O IgA肾病 母子 3 血液透析 6 例22 女 59 B 男 30 O IgA肾病 母子 3 血液透析 12 例23 女 55 AB 男 33 A 慢性肾小球肾炎 母子 3 血液透析 7 -
[1] Zschiedrich S, Kramer-Zucker A, Jänigen B, et al. An update on ABO-incompatible kidney transplantation[J]. Transpl Int, 2015, 28(4): 387-397. doi: 10.1111/tri.12485
[2] Crew RJ, Ratner LE. ABO-incompatible kidney transplantation: current practice and the decade ahead[J]. Curr Opin Organ Transplant, 2010, 15(4): 526-530. doi: 10.1097/MOT.0b013e32833bfbba
[3] Okumi M, Toki D, Nozaki T, et al. ABO-Incompatible Living Kidney Transplants: Evolution of Outcomes and Immunosuppressive Management[J]. Am J Transplant, 2016, 16(3): 886-896. doi: 10.1111/ajt.13502
[4] 李金锋, 张浩杰, 丰贵文, 等. 以输尿管为导向的后腹腔镜活体供肾切取术的临床研究[J]. 临床泌尿外科杂志, 2018, 33(11): 883-886, 893. https://lcmw.chinajournal.net.cn/WKC/WebPublication/paperDigest.aspx?paperID=6f4d04d7-36c2-4797-bc5f-099487487e4e
[5] 李金锋, 罗永胜, 张浩杰, 等. ABO血型不相容肾移植5例临床报告并文献复习[J]. 临床泌尿外科杂志, 2020, 35(1): 30-35. https://lcmw.chinajournal.net.cn/WKC/WebPublication/paperDigest.aspx?paperID=89c6c18f-04e6-4452-a44a-69ab81512172
[6] Avery RK, Motter JD, Jackson KR, et al. Quantifying infection risks in incompatible living donor kidney transplant recipients[J]. Am J Transplant, 2021, 21(4): 1564-1575. doi: 10.1111/ajt.16316
[7] Morath C, Zschiedrich S, Speer C, et al. Clinical outcomes after ABO-incompatible renal transplantation[J]. Lancet, 2019, 394(10213): 1989.
[8] Pavenski K, Bucholz M, Cheatley PL, et al. The First North American Experience Using Glycosorb Immunoadsorption Columns for Blood Group-Incompatible Kidney Transplantation[J]. Can J Kidney Health Dis, 2020, 7: 2054358120962586.
[9] Takahashi K, Saito K. ABO-incompatible kidney transplantation[J]. Transplant Rev-Orlan, 2013, 27(1): 1-8. doi: 10.1016/j.trre.2012.07.003
[10] Currie IS, Henderson LK. ABO-incompatible renal transplantation[J]. Lancet, 2019, 393(10185): 2014-2016. doi: 10.1016/S0140-6736(19)30296-X
[11] Uchida J, Kosoku A, Naganuma T, et al. Latest insights on ABO-incompatible living-donor renal transplantation[J]. Int J Urol, 2020, 27(1): 30-38. doi: 10.1111/iju.14109
[12] 汪昶, 陈立中, 邱江, 等. ABO血型不合活体肾移植11例分析[J]. 器官移植, 2019, 10(2): 182-186. doi: 10.3969/j.issn.1674-7445.2019.02.011
[13] 王显丁, 邱阳, 宋涂润, 等. ABO血型不相容亲属活体肾移植14例报告[J]. 中华器官移植杂志, 2016, 37(6): 348-352. doi: 10.3760/cma.j.issn.0254-1785.2016.06.007
[14] 王显丁, 邱阳, 宋涂润, 等. ABO血型不相容亲属活体肾移植的个体化预处理[J]. 中华器官移植杂志, 2015, 36(8): 449-452. doi: 10.3760/cma.j.issn.0254-1785.2015.08.001
[15] 蒋鸿涛, 李涛, 任坤, 等. ABO血型不相容亲属活体肾移植的多中心研究[J]. 中华器官移植杂志, 2020, 41(5): 259-264. doi: 10.3760/cma.j.cn421203-20200416-00120
[16] Okada M, Watarai Y, Iwasaki K, et al. Favorable results in ABO-incompatible renal transplantation without B cell-targeted therapy: Advantages and disadvantages of rituximab pretreatment[J]. Clin Transplant, 2017, 31(10): e13071.
[17] Tran L, Baars JW, Aarden L, et al. Pharmacokinetics of rituximab in patients with CD20 positive B-cell malignancies[J]. Hum Antibodies, 2010, 19(1): 7-13. doi: 10.3233/HAB-2010-0215
[18] Tran L, Baars JW, de Boer JP, et al. The pharmacokinetics of 131I-rituximab in a patient with CD20 positive non-Hodgkin Lymphoma: evaluation of the effect of radioiodination on the biological properties of rituximab[J]. Hum Antibodies, 2011, 20(1-2): 37-40. doi: 10.3233/HAB-2011-0240
[19] Genberg H, Hansson A, Wernerson A, et al. Pharmacodynamics of rituximab in kidney transplantation[J]. Transplantation, 2007, 84(12 Suppl): S33-36.
[20] Tomita Y, Iwadoh K, Ogawa Y, et al. Single fixed low-dose rituximab as induction therapy suppresses de novo donor-specific anti-HLA antibody production in ABO compatible living kidney transplant recipients[J]. PLoS One, 2019, 14(10): e0224203. doi: 10.1371/journal.pone.0224203
[21] Krishnan N, Coates R, Daga S, et al. ABO-incompatible renal transplantation without antibody removal using conventional immunosuppression alone[J]. Am J Transplant, 2015, 15(6): 1728-1729. doi: 10.1111/ajt.13255
[22] Krishnan N, Higgins R, Short A, et al. Kidney Transplantation Significantly Improves Patient and Graft Survival Irrespective of BMI: A Cohort Study[J]. Am J Transplant, 2015, 15(9): 2378-2386. doi: 10.1111/ajt.13363
[23] Lo P, Sharma A, Craig JC, et al. Preconditioning Therapy in ABO-Incompatible Living Kidney Transplantation: A Systematic Review and Meta-Analysis[J]. Transplantation, 2016, 100(4): 933-942. doi: 10.1097/TP.0000000000000933
[24] Takahashi K. Recent findings in ABO-incompatible kidney transplantation: classification and therapeutic strategy for acute antibody-mediated rejection due to ABO-blood-group-related antigens during the critical period preceding the establishment of accommodation[J]. Clin Exp Nephrol, 2007, 11(2): 128-141. doi: 10.1007/s10157-007-0461-z
[25] Takahashi K, Saito K, Nakagawa Y, et al. Mechanism of acute antibody-mediated rejection in ABO-incompatible kidney transplantation: which anti-A/anti-B antibodies are responsible, natural or de novo?[J]. Transplantation, 2010, 89(5): 635-637. doi: 10.1097/TP.0b013e3181c89307
-




 下载:
下载: