Analysis of risk factors of benign prostatic hyperplasia complicated with detrusor underactivity and establishment of risk nomogram prediction model
-
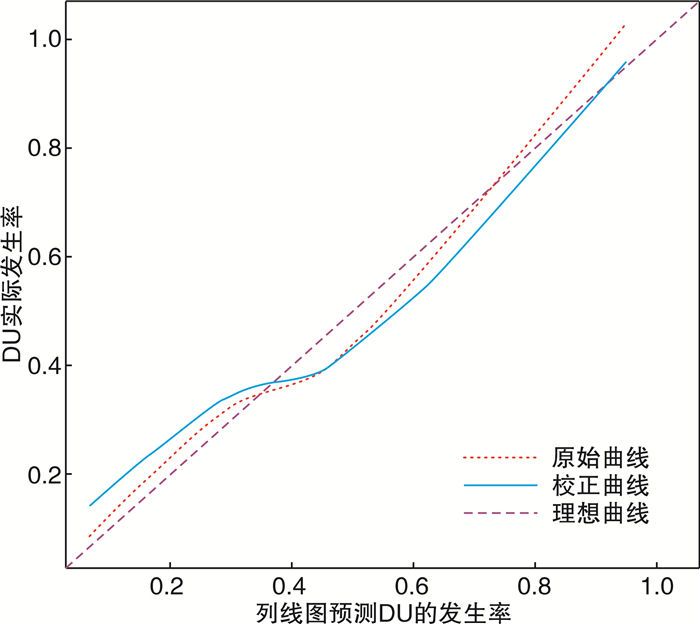
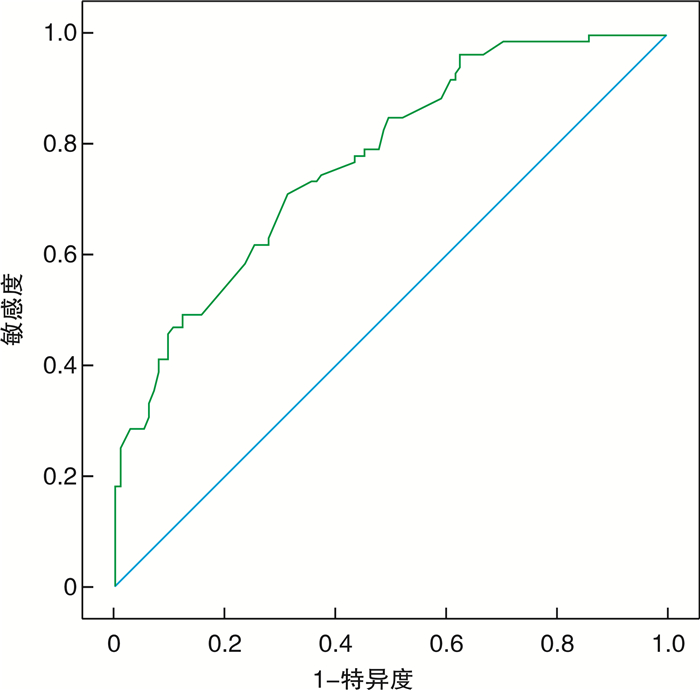
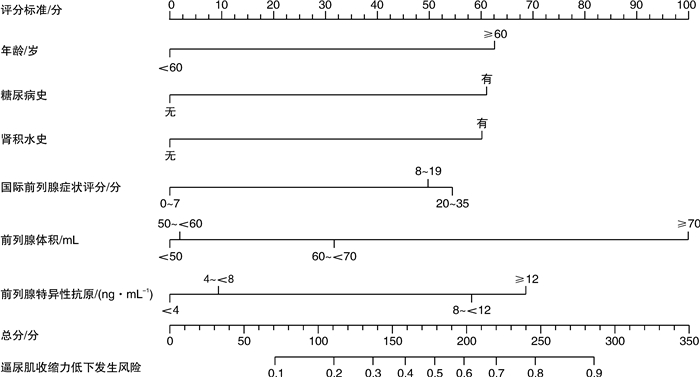
摘要: 目的 探讨良性前列腺增生(BPH)并发逼尿肌活动低下(DU)的危险因素,并构建列线图预测模型。方法 选取2019年6月—2021年6月于广州市中西医结合医院就诊的202例BPH患者作为研究对象,收集患者的临床资料,使用logistic回归分析BPH患者并发DU的危险因素,并建立列线图预测模型。结果 年龄≥60岁、糖尿病史、肾积水史、国际前列腺症状评分(IPSS)高、前列腺体积(PV)大和前列腺特异性抗原(PSA)水平高是BPH患者并发DU的独立危险因素(P < 0.05)。依此建立预测BPH患者并发DU的列线图风险模型,模型验证结果显示C-index为0.807,校正曲线趋近于理想曲线,ROC的曲线下面积(AUC)为0.790(95%CI:0.767~0.831),表明该模型具有良好的预测能力。结论 BPH并发DU的危险因素包括年龄≥60岁、糖尿病史、肾积水史、IPSS评分高、PV大和PSA水平高,据此构建的列线图模型能准确预测BPH患者并发DU的风险概率。Abstract: Objective To investigate the risk factors of detrusor underactivity (DU) in benign prostatic hyperplasia (BPH), and to construct a nomogram prediction model.Methods From June 2019 to June 2021, 202 patients with BPH treated in Guangzhou Integrated Traditional Chinese and Western Medicine Hospital were selected as the research objects. The clinical data of patients were collected. The risk factors of BPH patients complicated with DU were analyzed by logistic regression, and the nomogram prediction model was established.Results Age over 60 years, history of diabetes, history of hydronephrosis, high IPSS score, large PV and high PSA level were independent risk factors for DU in BPH patients (P < 0.05). A nomogram risk model for predicting DU in patients with BPH was established. The model verification results showed that the C-index was 0.807. The correction curve was close to the ideal curve, and the AUC of ROC curve was 0.790 (95%CI: 0.767-0.831), indicating that the model has good prediction ability.Conclusion Risk factors of DU in BPH patients include age over 60 years, diabetes history, hydronephrosis history, high IPSS score, high PV and high PSA level. Based on this, the nomogram model can accurately predict the risk probability of DU in BPH patients.
-
Key words:
- benign prostatic hyperplasia /
- detrusor underactivity /
- risk factors /
- nomogram
-

-
表 1 BPH患者并发DU的单因素分析
例(%),X±S 项目 DU组(n=87) 非DU组(n=115) χ2/t P 年龄/岁 8.498 0.004 < 60 8 29 ≥60 79 86 BMI 0.506 0.477 < 24 73 92 ≥24 14 23 吸烟史 26 37 0.121 0.728 糖尿病史 21 10 9.091 0.003 高血压病史 25 32 0.020 0.887 尿潴留史 56 62 2.229 0.135 肾积水史 16 7 7.431 0.006 IPSS评分/分 10.275 0.006 0~7 12 38 8~19 52 57 20~35 23 20 PV/mL 13.233 0.004 < 50 11 24 50~ < 60 24 46 60~ < 70 37 40 ≥70 15 5 PSA水平/(ng·mL-1) 21.035 < 0.001 < 4 2 5 4~ < 8 22 64 8~ < 12 48 36 ≥12 15 10 逼尿肌过度活动 19 24 0.028 0.868 膀胱初感觉时的膀胱容量/mL 138.47±60.24 146.09±62.15 0.874 0.383 排尿量/mL 165.83±102.64 175.82±108.20 0.664 0.507 残余尿量/mL 77.27±56.82 83.54±58.05 0.767 0.444 表 2 BPH患者并发DU的多因素logistic回归分析
项目 回归系数 SE Waldχ2 P OR 95%CI 年龄 1.395 0.484 8.311 0.004 4.034 1.563~10.412 糖尿病史 1.320 0.484 7.427 0.006 3.744 1.449~9.676 肾积水史 1.189 0.563 4.463 0.035 3.283 1.090~9.891 IPSS评分 0.597 0.249 5.750 0.016 1.817 1.115~2.961 PV 0.591 0.196 9.096 0.003 1.806 1.230~2.652 PSA水平 0.692 0.232 8.912 0.003 1.999 1.268~3.149 常量 -4.357 0.743 34.358 < 0.001 0.013 - -
[1] 康健, 管雯斌, 朱自强, 等. 核磁共振成像对良性前列腺增生组织成分的预测研究[J]. 临床泌尿外科杂志, 2020, 35(5): 367-370. https://www.cnki.com.cn/Article/CJFDTOTAL-LCMW202005008.htm
[2] Chughtai B, Forde JC, Thomas DD, et al. Benign Prostatic Hyperplasia[J]. Neurourol Urodyn, 2016, 2: 16031.
[3] Thomas D, Zorn KC, Zaidi N, et al. Does urodynamics predict voiding after benign prostatic hyperplasia surgery in patients with detrusor underactivity?[J]. Asian J Urol, 2019, 6(3): 264-269. doi: 10.1016/j.ajur.2018.12.005
[4] Luo F, Sun HH, Su YH, et al. Assessment of noninvasive predictors of bladder detrusor underactivity in BPH/LUTs patients[J]. Int Urol Nephrol, 2017, 49(5): 787-792. doi: 10.1007/s11255-017-1539-5
[5] Dong YM, Sun J, Li YX, et al. Development and Validation of a Nomogram for Assessing Survival in Patients With COVID-19 Pneumonia[J]. Clin Infect Dis, 2021, 72(4): 652-660. doi: 10.1093/cid/ciaa963
[6] Fishburn SJ, Mullins ME. A simple approximation of the QT nomogram[J]. Clin Toxicol(Phila), 2021, 59(2): 177-178. doi: 10.1080/15563650.2020.1768267
[7] 那彦群. 中国泌尿外科疾病诊断治疗指南手册: 2014版[M]. 北京: 人民卫生出版社, 2014: 245-265.
[8] Rosier PF, Schaefer W, Lose G, et al. International Continence Society Good Urodynamic Practices and Terms 2016: Urodynamics, uroflowmetry, cystometry, and pressure-flow study[J]. Neurourol Urodyn, 2017, 36(5): 1243-1260. doi: 10.1002/nau.23124
[9] 廖利民. 尿动力学[M]. 北京: 人民军医出版社, 2012: 159-194.
[10] 张亚龙, 高继学, 张烨. 良性前列腺增生症患者膀胱壁和逼尿肌厚度改变的相关研究进展[J]. 新医学, 2017, 48(10): 688-691. doi: 10.3969/j.issn.0253-9802.2017.10.003
[11] 廖凯, 沈华, 吴伟力, 等. 逼尿肌过度活动伴收缩力受损患者尿动力学分析与治疗效果评价[J]. 现代泌尿外科杂志, 2019, 24(7): 550-554. doi: 10.3969/j.issn.1009-8291.2019.07.007
[12] 任宝明, 马龙, 闵晓明. 不同年龄前列腺增生患者下尿路症状的相关性分析[J]. 疑难病杂志, 2019, 18(2): 167-169, 174. doi: 10.3969/j.issn.1671-6450.2019.02.015
[13] 刘亚东, 卢晓明, 周国洋, 等. 前列腺增生合并糖尿病患者下尿路症状特点尿动力学分析[J]. 中华全科医师杂志, 2018, 17(12): 1006-1008. doi: 10.3760/cma.j.issn.1671-7368.2018.12.011
[14] 陶森. 预判前列腺增生患者逼尿肌收缩力减弱的相关因素分析[D]. 长春: 吉林大学, 2018.
[15] Schifano N, Capogrosso P, Matloob R, et al. Patients presenting with lower urinary tract symptoms who most deserve to be investigated for primary bladder neck obstruction[J]. Sci Rep, 2021, 11(1): 4167. doi: 10.1038/s41598-021-83672-5
[16] 沈立新. 良性前列腺增生的超声学参数与膀胱出口梗阻的相关性分析[J]. 重庆医学, 2019, 48(19): 3314-3317. doi: 10.3969/j.issn.1671-8348.2019.19.018
[17] 刘丹丹, 陈敏, 韩晓敏, 等. 不同梗阻程度下前列腺增生患者的尿动力学分析[J]. 临床泌尿外科杂志, 2018, 33(9): 730-733, 737. https://www.cnki.com.cn/Article/CJFDTOTAL-LCMW201809013.htm
[18] Kusuma Duarsa GW, Sari YA, Gde Oka AA, et al. Serum testosterone and prostate-specific antigen levels are major risk factors for prostatic volume increase among benign prostatic hyperplasia patients[J]. Asian J Urol, 2021, 8(3): 289-297. doi: 10.1016/j.ajur.2020.06.001
[19] 王文振, 刘玉强, 俎树禄, 等. 良性前列腺增生并发急性尿潴留患者的逼尿肌收缩功能[J]. 山东大学学报(医学版), 2018, 56(3): 66-71. https://www.cnki.com.cn/Article/CJFDTOTAL-SDYB201803012.htm
[20] 仝姗姗, 毛婷婷, 张莹莹, 等. 良性前列腺增生继发急性尿潴留的危险因素分析及预测模型构建[J]. 微创泌尿外科杂志, 2021, 10(1): 61-64. https://www.cnki.com.cn/Article/CJFDTOTAL-WCMN202101015.htm
-




 下载:
下载: