Diagnosis and treatment of initial urachal carcinoma: a single-center study of 55 cases
-
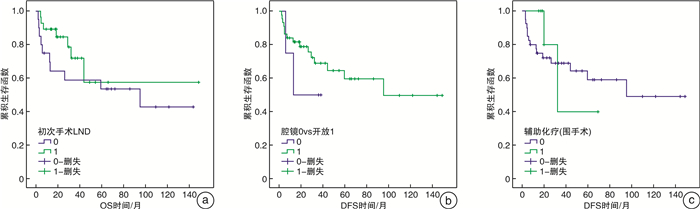
摘要: 目的探讨脐尿管癌的治疗模式与治疗效果。方法筛选2006年1月—2021年1月在中山大学附属肿瘤医院接受初次手术治疗的脐尿管癌患者。收集其临床病理资料及预后信息,Kaplan-Meier法评估患者的生存时间,Cox多因素回归分析与生存预后相关的独立预测因子。结果总共55例患者,其中男40例,女15例,中位年龄为47岁,所有患者均为Sheldon分期Ⅲ~Ⅳ期。中位随访时间为36个月,17例患者出现复发。Sheldon分期和复发是总生存的独立预测因子(P < 0.001)。淋巴结清扫和开放手术可能与无瘤生存时间相关,虽然这些获益差异无统计学意义。结论脐尿管癌是一种罕见的恶性肿瘤,Sheldon分期和复发与患者的长期生存有关。尽管本研究显示淋巴结清扫术不是脐尿管癌预后的独立危险因素,但我们认为它有利于准确分期,能够改善脐尿管癌患者的预后。Abstract: ObjectiveTo explore the treatment model and treatment effects of urachal carcinoma.MethodsFrom January 2006 to January 2021, patients who had been diagnosed with urachal carcinoma and received initial surgical treatment at Sun Yat-sen University Cancer Center were screened. The clinical pathological data and follow-up information were collected. The Kaplan-Meier method was used to assess the survival time and multivariate Cox regression was used to analyze the independent prognostic factors that were related to the survival of patients.ResultsOf the 55 patients, 40 were males and 15 were females. Their median age was 47 years old, and they were all in stage Ⅲ-Ⅳ (Sheldon stage). The median follow-up period was 36 months, and 17 patients have developed recurrence. Sheldon stage and recurrence were independent predictors of overall survival (P < 0.001). Lymph node dissection and open surgery might be associated with tumor-free survival time, but these differences were not statistically significant.ConclusionUrachal carcinoma is a rare bladder malignant neoplasm, and Sheldon stage and recurrence were associated with long-term survival. Although lymph node dissection was not an independent risk factor for the prognosis of urachal carcinomas in this study, we thought it was conducive to accurate staging and improvement of patients' prognosis.
-
Key words:
- urachal carcinoma /
- survival analysis /
- partial cystectomy /
- lymph node dissection
-

-
表 1 脐尿管癌总生存危险因素分析
因素 单因素 多因素 P Wald HR(95%CI) P 年龄(> 50岁vs ≤50岁) 0.470 性别(男vs女) 0.889 肿瘤大小(> 3 cm vs ≤3 cm) 0.657 Sheldon分期(Ⅳ期vs Ⅲ期) < 0.001 22.7 25.1(6.7~94.3) < 0.001 分级(高vs中低) 0.128 腔镜手术(是vs否) 0.387 淋巴结清扫(是vs否) 0.788 术后复发(是vs否) < 0.001 18.4 15.4(4.4~53.9) < 0.001 -
[1] Elser C, Sweet J, Cheran SK, et al. A case of metastatic urachal adenocarcinoma treated with several different chemotherapeutic regimens[J]. Can Urol Assoc J, 2012, 6(1): E27-E31.
[2] Yasui M, Jikuya R, Tatenuma T, et al. Urachal Carcinoma with Peritoneal Dissemination Treated with Chemotherapy and Surgical Resection Leading to Prolonged Survival with No Recurrence[J]. Case Rep Urol, 2018, 2018: 9836154.
[3] Siefker-Radtke A. Urachal adenocarcinoma: a clinician's guide for treatment[J]. Semin Oncol, 2012, 39(5): 619-624. doi: 10.1053/j.seminoncol.2012.08.011
[4] Piégay F, Mornex JF. Combined modalities treatment of pulmonary metastasis from an urachal adenocarcinoma[J]. Rare Tumors, 2013, 5(3): e32.
[5] Wright JL, Porter MP, Li CI, et al. Differences in survival among patients with urachal and nonurachal adenocarcinomas of the bladder[J]. Cancer, 2006, 107(4): 721-728. doi: 10.1002/cncr.22059
[6] Mardi K, Gupta N. Urachal papillary cystadenocarcinoma: a rare case report[J]. J Cancer Res Ther, 2011, 7(2): 223-225. doi: 10.4103/0973-1482.82934
[7] Besarani D, Purdie CA, Townell NH. Recurrent urachal adenocarcinoma[J]. J Clin Pathol, 2003, 56(11): 882. doi: 10.1136/jcp.56.11.882
[8] Quan J, Pan X, Jin L et al. Urachal carcinoma: Report of two cases and review of the literature[J]. Mol Clin Oncol, 2017, 6(1): 101-104. doi: 10.3892/mco.2016.1082
[9] 杨洋, 张晓卿, 肖云翔, 等. 脐尿管癌的诊疗经验和预后分析[J]. 中华泌尿外科杂志, 2020, 41(10): 741-745. doi: 10.3760/cma.j.cn112330-20200520-00407
[10] Ashley RA, Inman BA, Sebo TJ, et al. Urachal carcinoma: clinicopathologic features and long-term outcomes of an aggressive malignancy[J]. Cancer, 2006, 107(4): 712-720. doi: 10.1002/cncr.22060
[11] Jia Z, Chang X, Li X, et al. Urachal Carcinoma: Are Lymphadenectomy and Umbilectomy Necessary?[J]. Med Sci Monit, 2020, 26: e927913.
[12] Bruins HM, Visser O, Ploeg M, et al. The clinical epidemiology of urachal carcinoma: results of a large, population based study[J]. J Urol, 2012, 188(4): 1102-1107. doi: 10.1016/j.juro.2012.06.020
[13] Siefker-Radtke AO, Gee J, Shen YU, et al. Multimodality Management of Urachal Carcinoma: The M.D. Anderson Cancer Center Experience[J]. J Urol, 2003, 169(4): 1295-1298. doi: 10.1097/01.ju.0000054646.49381.01
[14] Herr HW, Bochner BH, Sharp D, et al. Urachal Carcinoma: Contemporary Surgical Outcomes[J]. J Urol, 2007, 178(1): 74-78. doi: 10.1016/j.juro.2007.03.022
[15] 柯春锦, 杨春光, 曾星, 等. 15例脐尿管癌的临床特征及预后分析[J]. 临床泌尿外科杂志, 2020, 35(4): 307-311. https://www.cnki.com.cn/Article/CJFDTOTAL-LCMW202004012.htm
[16] Maurer A, Ortiz-Bruechle N, Guricova K, et al. Comparative genomic profiling of glandular bladder tumours[J]. Virchows Arch, 2020, 477(3): 445-454. doi: 10.1007/s00428-020-02787-8
[17] Szarvas T, Módos O, Niedworok C, et al. Clinical, prognostic, and therapeutic aspects of urachal carcinoma-A comprehensive review with meta-analysis of 1, 010 cases[J]. Urol Oncol, 2016, 34(9): 388-398. doi: 10.1016/j.urolonc.2016.04.012
[18] Collazo-Lorduy A, Castillo-Martin M, Wang L, et al. Urachal Carcinoma Shares Genomic Alterations with Colorectal Carcinoma and May Respond to Epidermal Growth Factor Inhibition[J]. Eur Urol, 2016, 70(5): 771-775. doi: 10.1016/j.eururo.2016.04.037
-




 下载:
下载: