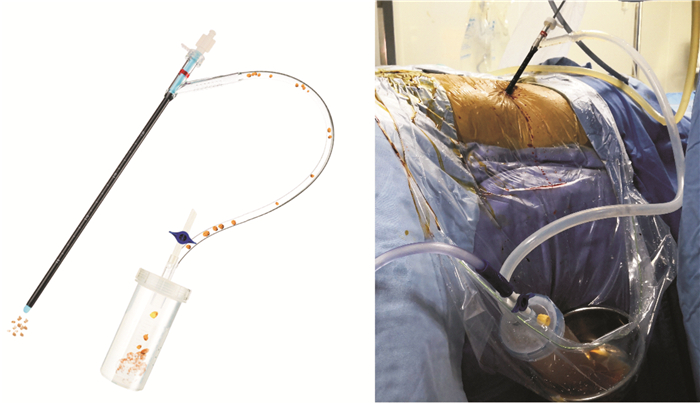
Application of ClearPetra access sheath with vacuum suction on percutaneous nephrolithotomy for complex kidney stones
-
摘要: 目的 探讨负压清石辅助工具配合钬激光在经皮肾镜取石术治疗复杂性肾结石中的应用价值。方法 回顾性分析2018年8月—2021年7月在华中科技大学同济医学院附属同济医院行单通道(F20)经皮肾镜取石术的96例复杂性肾结石患者资料。根据术中是否应用负压清石辅助工具分为负压组(47例)和对照组(49例)。所有手术均采用超声引导经12肋下或11肋间穿刺目标盏或结石,建立20F经皮肾手术通道,并采用钬激光碎石。统计所有患者基本资料、手术相关参数、术后主要并发症发生率等数据。结果 所有患者均顺利完成手术。负压组患者年龄大于对照组。负压组与对照组的性别、体重指数(BMI)、是否合并糖尿病、术前尿培养阳性史占比、结石最长径、手术时长等指标差异均无统计学意义。2组术后输血率、结石清除率差异无统计学意义。负压组术后全身炎症反应综合征(SIRS)的发生率低于对照组(2.12% vs 16.33%,P=0.042),且负压组术后恢复时间更短[(5.04±1.37) d vs (6.16±1.51) d,P < 0.01]。负压组术后血常规白细胞基本正常比例显著高于对照组(95.74% vs 73.47%,P=0.004),多因素分析显示使用负压清石辅助工具是术后血常规白细胞正常与否的独立影响因素。结论 对于复杂性肾结石,应用负压清石辅助工具有助于减少经皮肾镜碎石取石术术后感染相关并发症发生,从而促进患者快速恢复。Abstract: Objective To explore the effect of ClearPetra access sheath with vacuum suction combined with holmium laser on percutaneous nephrolithotomy in the treatment of complex kidney stones.Methods The data of 96 patients with complex kidney stones who underwent single-tract percutaneous nephrolithotomy in Tongji Hospital from August 2018 to July 2021 were retrospectively analyzed. According to whether ClearPetra access sheath with vacuum suction was used during the operation, they were divided into vacuum suction group (n=47) and control group (n=49). In all operations, ultrasound guidance was used to puncture the target calyx or calculus via the 12 subcostal or 11 intercostal area to establish a 20F percutaneous surgical tract, and the holmium laser was used for stone crushing. Basic data of all patients, operation-related parameters, incidence of major postoperative complications and other data were analyzed.Results All the included cases were successfully performed the operation. Patients in the vacuum suction group were older than those in the control group. There were no statistical differences between the vacuum suction and the control group in terms of gender ratio, BMI, diabetes mellitus, the proportion of positive urine culture history, the size of stones, operation time or other parameters. There was no statistical difference in the rate of blood transfusion or stone free rates between the two groups. The incidence of systemic inflammatory response syndrome (SIRS) in the vacuum suction group was lower than that in the control group (2.12% vs 16.33%, P=0.042), and the recuperation time in the vacuum suction group was shorter ([5.04±1.37] days vs [6.16±1.51] days, P < 0.01). The proportion of normal white blood cells in the vacuum suction group was significantly higher than that in the control group (95.74% vs 73.47%, P=0.004). Multivariate analysis showed that the use of ClearPetra access sheath with vacuum suction was an independent factor to predict the postoperative changes of white blood cells.Conclusion The use of ClearPetra access sheath with vacuum suction can reduce the incidence of infection-related complications after percutaneous nephrolithotomy for complex kidney stones, and promote rapid recovery of patients.
-

-
表 1 2组患者基线资料
例,X±S 项目 负压组
(47例)对照组
(49例)P值 年龄/岁 57.64±9.99 52.69±13.65 0.046 男/女 15/32 24/25 0.135 右/左 34/13 25/24 0.053 BMI/(kg·m-2) 24.10±3.02 23.68±4.10 0.572 合并糖尿病 5 4 0.948 术前尿培养阳性史(+/-) 8/39 8/41 0.855 结石长径/cm 4.80±1.34 5.40±2.82 0.182 表 2 2组患者手术相关情况比较
X±S 项目 负压组(47例) 对照组(49例) P值 手术时长/min 100.30±29.82 106.65±37.85 0.364 结石清除/例(%) 28(59.57) 23(46.94) 0.300 术后恢复时间/d 5.04±1.37 6.16±1.51 <0.001 表 3 2组患者PCNL术后血常规情况及并发症比较
例(%) 项目 负压组(47例) 对照组(49例) P值 术后血常规白细胞计数基本正常 45(95.74) 36(73.47) 0.004 并发症 体温异常 2(4.26) 5(10.20) 0.467 SIRS 1(2.12) 8(16.33) 0.042 脓毒症 0(0) 3(6.12) 0.256 感染性休克 0(0) 0(0) - 输血 0(0) 3(6.12) 0.256 血管造影/栓塞 0(0) 0(0) - 表 4 影响术后血常规白细胞计数的多因素回归分析
变量 B SE χ2 P值 Exp(B) 95%CI 年龄 0.060 0.028 4.422 0.035 1.062 1.004~1.123 性别 -0.790 0.817 0.935 0.334 0.454 0.091~2.251 BMI 0.056 0.091 0.374 0.541 1.058 0.884~1.265 合并糖尿病 -0.316 1.050 0.091 0.763 0.729 0.093~5.709 尿培养阳性史 0.008 0.915 0.000 0.993 1.008 0.168~6.056 结石最长径 0.279 0.194 2.062 0.151 1.322 0.903~1.935 手术时间 -0.010 0.009 1.091 0.296 0.990 0.972~1.009 是否使用负压 -1.904 0.824 5.344 0.021 0.149 0.030~0.748 常量 -1.188 3.445 0.119 0.730 0.305 -
[1] Desai M, Jain P, Ganpule A, et al. Developments in technique and technology: the effect on the results of percutaneous nephrolithotomy for staghorn calculi[J]. BJU Int, 2009, 104(4): 542-548;discussion 548. doi: 10.1111/j.1464-410X.2009.08472.x
[2] de la Rosette JJ, Opondo D, Daels FP, et al. Categorisation of complications and validation of the Clavien score for percutaneous nephrolithotomy[J]. Eur Urol, 2012, 62(2): 246-255. doi: 10.1016/j.eururo.2012.03.055
[3] Gadzhiev N, Malkhasyan V, Akopyan G, et al. Percutaneous nephrolithotomy for staghorn calculi: Troubleshooting and managing complications[J]. Asian J Urol, 2020, 7(2): 139-148. doi: 10.1016/j.ajur.2019.10.004
[4] Zhu Z, Cui Y, Zeng H, et al. Suctioning versus traditional minimally invasive percutaneous nephrolithotomy to treat renal staghorn calculi: A case-matched comparative study[J]. Int J Surg, 2019, 72: 85-90. doi: 10.1016/j.ijsu.2019.10.032
[5] Tokas T, Herrmann T, Skolarikos A, et al. Pressure matters: intrarenal pressures during normal and pathological conditions, and impact of increased values to renal physiology[J]. World J Urol, 2019, 37(1): 125-131. doi: 10.1007/s00345-018-2378-4
[6] 冯大林, 崔韵, 张军晖, 等. 经皮肾镜取石术后全身炎症反应综合征的危险因素分析[J]. 临床泌尿外科杂志, 2021, 36(4): 259-263. https://www.cnki.com.cn/Article/CJFDTOTAL-LCMW202104002.htm
[7] 余虓, 夏丁, 彭鄂军, 等. 超声引导下SVOF原则两步穿刺法建立经皮肾镜工作通道的临床研究[J]. 中华外科杂志, 2018, 56(10): 764-767.
[8] Shankar-Hari M, Phillips GS, Levy ML, et al. Developing a New Definition and Assessing New Clinical Criteria for Septic Shock: For the Third International Consensus Definitions for Sepsis and Septic Shock(Sepsis-3)[J]. JAMA, 2016, 315(8): 775-787. doi: 10.1001/jama.2016.0289
[9] 张加桥, 余虓, 姚炜敏, 等. 使用负压清石鞘对经皮肾镜碎石术术后感染相关并发症的影响[J]. 现代泌尿外科杂志, 2020, 25(2): 156-158, 161. https://www.cnki.com.cn/Article/CJFDTOTAL-MNWK202002016.htm
[10] He Z, Tang F, Lei H, et al. Risk factors for systemic inflammatory response syndrome after percutaneous nephrolithotomy[J]. Prog Urol, 2018, 28(12): 582-587. doi: 10.1016/j.purol.2018.06.006
[11] Chen D, Jiang C, Liang X, et al. Early and rapid prediction of postoperative infections following percutaneous nephrolithotomy in patients with complex kidney stones[J]. BJU Int, 2019, 123(6): 1041-1047. doi: 10.1111/bju.14484
[12] Tan F, Gan X, Deng Y, et al. Intraoperative dexmedetomidine attenuates postoperative systemic inflammatory response syndrome in patients who underwent percutaneous nephrolithotomy: a retrospective cohort study[J]. Ther Clin Risk Manag, 2018, 14: 287-293. doi: 10.2147/TCRM.S157320
[13] Abourbih S, Alsyouf M, Yeo A, et al. Renal Pelvic Pressure in Percutaneous Nephrolithotomy: The Effect of Multiple Tracts[J]. J Endourol, 2017, 31(10): 1079-1083. doi: 10.1089/end.2017.0298
-




 下载:
下载: