-
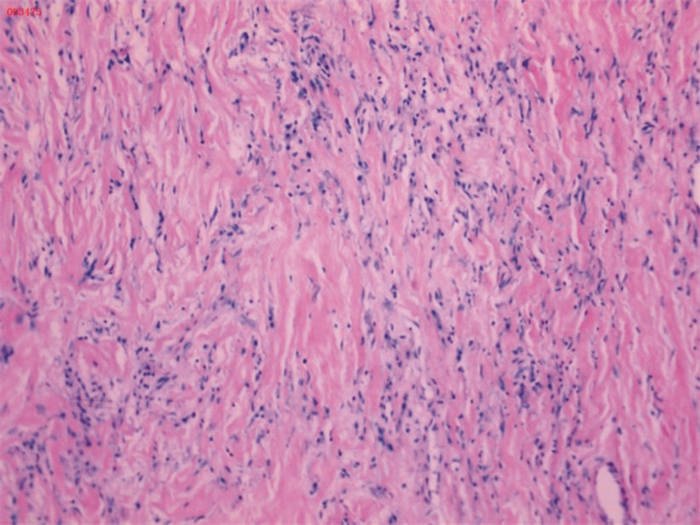
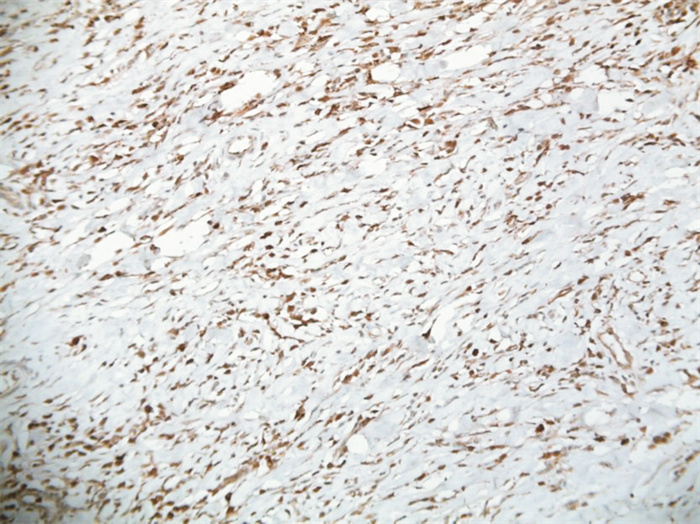
摘要: 分析2例儿童睾丸旁炎性肌纤维母细胞瘤患者资料并复习文献。例1,男,7岁。主诉发现左侧阴囊肿物1个月,B超显示左侧睾丸旁实性肿物。例2,男,9岁。主诉右侧阴囊肿大疼痛1个月,B超显示右侧睾丸背上方实性肿块,范围约3.0 cm×1.9 cm×1.4 cm。2例肿瘤均完整切除,例1标本光镜下肿瘤细胞为纤维组织、胶原纤维中间散在淋巴细胞、浆细胞,可见淋巴滤泡形成,免疫组化:ALK(-),desmin部分(+),SMA(+),CD68散在(+),calretinin(-),S-100(-)。诊断为炎性肌纤维母细胞瘤。例2标本光镜下肿瘤细胞大部分为纤维血管组织,表面无包膜,部分为成纤维细胞,其间可见散在及灶状炎细胞浸润,一侧可见附睾管。免疫组化:SMA(+)、Ki67(+)约为2%。诊断为附睾炎性肌纤维母细胞瘤。术后3个月B超复查,例1随诊4年未见复发,例2失访。Abstract: The data of two children with paratesticular inflammatory myofibroblastoma were analyzed and the related literature was reviewed. Case 1 was a 7-year-old boy. He complained that the left scrotal mass was found for one month, and ultrasound showed the solid mass near the left testicle. Example 2 was a 9-year-old boy. He complained of swelling and pain of the right scrotum for one month. Ultrasound showed a solid mass above the dorsum of the right testis, with a range of 3.0 cm×1.9 cm× 1.4 cm. The tumors were completely removed in two cases. Pathological findings of the first case showed that the tumor cells were fibrous tissues, and there were scattered lymphocytes and plasma cells in the middle of collagen fibers, in which lymphoid follicles could be seen. Immunohistochemistry stain showed ALK(-), desmin part(+), SMA(+), CD68 scattered (+), calretinin(-), S-100(-). The pathological diagnosis was inflammatory myofibroblastic tumor. The second case showed that most of the tumor cells were fibrous vascular tissue, with no capsule on the surface, and some were fibroblasts, in which scattered and focal inflammatory cell infiltration and the epididymal canal on one side could be seen. Immunohistochemistry stain showed SMA(+), Ki67(+) was about 2%. The pathological diagnosis was the inflammatory myofibroblastic tumor of epididymis. Ultrasound was taken every 3 months for both patients. The case 1 had no recurrence during 4 years of follow-up, and the case 2 lost follow-up.
-
Key words:
- paratesticular tumor /
- children /
- inflammatory myofibroblastic tumor
-

-
表 1 Pubmed检索近年来发表位于睾丸旁IMT情况
作者 年龄/岁 年份 杂志 部位 超声表现 肿物大小 手术 随访 Tunuguntla等[11] 17 2011 Urology 右侧阴
囊肿块右侧睾丸旁混杂回声肿块,实体和囊性成分延伸至附睾 6.0 cm×2.2 cm× 1.8 cm 肿物及右侧睾丸切除术 4年未见复发 Harel等[12] 17 2014 Case Rep Urol 右侧阴
囊肿块睾丸旁低回声,血流丰富不均匀肿块 0.7 cm×0.8 cm×0.6 cm 肿物切除术 3个月未见复发 Sönmez等[13] 14 2001 Journal of Pediatric Surgery 右侧阴
囊肿块右侧睾丸不规则增大 2.3 cm×2.3 cm 睾丸切除术 9个月未见复发 Vates等[14] 4 1993 Journal of Urology 左侧阴
囊肿块左侧睾丸旁实性肿块 2.5 cm×2.0 cm×1.0 cm 肿物切除术 5年未见复发 Vates等[14] 18 1993 Journal of Urology 右侧阴
囊肿块右侧睾丸旁肿块 3.0 cm×3.0 cm×2.0 cm 肿物切除术 5年未见复发 -
[1] Janik JS, Janik JP, Lovell MA, et al. Recurrent inflammatory pseudotumorsin children[J]. J Pediatr Surg, 2003, 38(10): 1491-1495. doi: 10.1016/S0022-3468(03)00501-3
[2] 杨星, 孙志熙, 刘涛, 等. 精索炎症性肌纤维母细胞瘤一例报告[J]. 中华泌尿外科杂志, 2010, 31(11): 785-785. doi: 10.3760/cma.j.issn.1000-6702.2010.11.019
[3] Gatto L, Del Gaudio M, Ravaioli M, et al. Paratesticular mesenchymal malignancies: a single-center case series, clinical management, and review of literature[J]. Integr Cancer Ther, 2020, 19: 1534735419900554.
[4] Zhao J, Han D, Gao M, et al. Inflammatory myofibroblastic tumor of the neck with thyroid invasion: a case report and literature review[J]. Gland Surg, 2020, 9(4): 1042-1047. doi: 10.21037/gs-20-355
[5] Di Ruscio V, Mastronuzzi A, Russo I, et al. Inflammatory myofibroblastic tumor of the upper airways harboring a new TRAF3-ALK fusion transcript[J]. Children(Basel), 2021, 8(6): 505.
[6] 徐雪莲, 叶云林, 郭胜杰, 等. 儿童睾丸良性肿瘤的临床分析[J]. 南方医科大学学报, 2014, 34(9): 1384-1385. https://www.cnki.com.cn/Article/CJFDTOTAL-DYJD201409032.htm
[7] Cooperman R, White B, Zincke JP, et al. Extratesticular inflammatory myofibroblastic tumor[J]. J Urol, 2003, 169(4): 1473. doi: 10.1097/01.ju.0000054925.34848.9c
[8] Coffin CM, Hornick JL, Fletcher CD. Inflammatory myofibroblastic tumor: comparison of clinicopathologic, histologic, and immunohistochemical features including ALK expression in atypical and aggressive cases[J]. Am J Surg Pathol, 2007, 31(4): 509-520. doi: 10.1097/01.pas.0000213393.57322.c7
[9] Bennett JA, Nardi V, Rouzbahman M, et al. Inflammatory myofibroblastic tumor of the uterus: a clinicopathological, immunohistochemical, and molecular analysis of 13 cases highlighting their broad morphologic spectrum[J]. Mod Pathol, 2017, 30(10): 1489-1503. doi: 10.1038/modpathol.2017.69
[10] Dangle PP, Wang WP, Pohar KS. Inflammatory myofibroblastic tumor of epididymis: a case report and review of literature[J]. World J Surg Oncol, 2008, 6: 119. doi: 10.1186/1477-7819-6-119
[11] Tunuguntla H, Mishra A, Jorda M, et al. Inflammatory myofibroblastic tumor of the epididymis: case report and review of the literature[J]. Urology, 2011, 78(1): 183-185. doi: 10.1016/j.urology.2010.09.027
[12] Harel M, Makari JH. Paratesticular inflammatory myofibroblastic tumor in a pediatric patient[J]. Case Rep Urol, 2014, 2014: 303678.
[13] Sönmez K, Türkyilmaz Z, Boyacioǧlu M, et al. Diffuse fibrous proliferation of tunica vaginalis associated with testicular infarction: a case report[J]. J Pediatr Surg, 2001, 36(7): 1057-1058. doi: 10.1053/jpsu.2001.24745
[14] Vates TS, Ruemmler-Fisch C, Smilow PC, et al. Benign fibrous testicular pseudotumors in children[J]. J Urol, 1993, 150(6): 1886-1888.
-

| 引用本文: | 解晓莹, 赵林胜, 裴广华, 等. 儿童睾丸旁炎性肌纤维母细胞瘤2例[J]. 临床泌尿外科杂志, 2023, 38(2): 157-160. doi: 10.13201/j.issn.1001-1420.2023.02.016 |
| Citation: | XIE Xiaoying, ZHAO Linsheng, PEI Guanghua, et al. Inflammatory myofibroblastic tumor of the paratestis[J]. J Clin Urol, 2023, 38(2): 157-160. doi: 10.13201/j.issn.1001-1420.2023.02.016 |
- Figure 1.
- Figure 2.
- Figure 3.



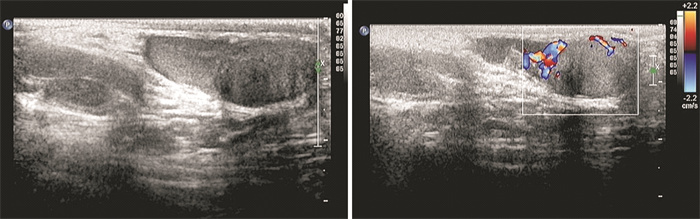
 下载:
下载: