Prognostic value of IMP3 and AGR in patients with non-muscular invasive bladder cancer after transurethral holmium laser resection
-
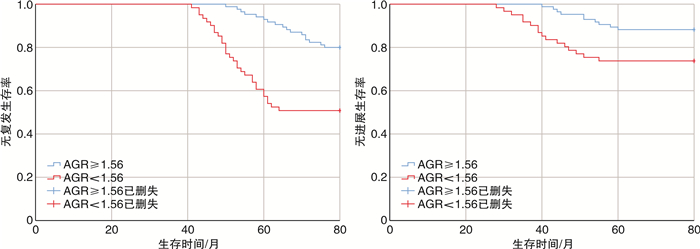
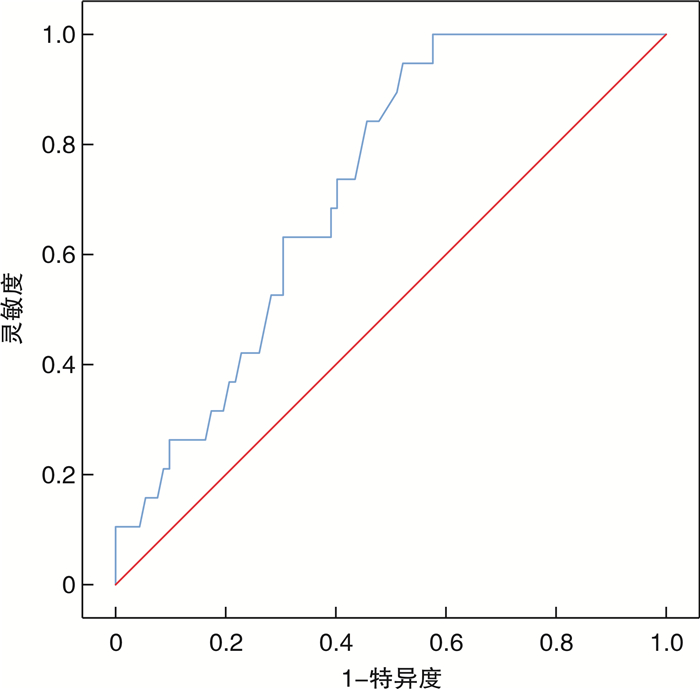
摘要: 目的 探讨胰岛素样生长因子ⅡmRNA结合蛋白族3(IMP3)与术前血清白蛋白/球蛋白比值(AGR)在非肌层浸润性膀胱癌(NMIBC)患者行经尿道钬激光切除术(HOLTUR)预后评估中的价值。方法 选取2016年1—12月我院接诊的146例NMIBC患者,术前检测血清AGR水平,收集患者癌组织及癌旁正常组织标本检测IMP3蛋白表达。随访5年,观察术后并发症发生情况。分析不同IMP3表达水平患者的临床特征和预后差异,应用ROC曲线和Kaplan-Meier生存曲线分析AGR的预后诊断价值,应用logistic回归分析预后不良的危险因素。结果 HOLTUR术后并发症总发生率为3.42%。癌组织中IMP3蛋白阳性表达率为67.12%(98/146),癌旁正常组织中未见IMP3蛋白阳性表达。不同IMP3表达水平患者病理组织分级、临床分期、复发情况等均差异有统计学意义(均P < 0.05)。癌组织IMP3阳性表达患者的5年生存率显著低于IMP3阴性表达患者(31.63% vs 60.42%,χ2=11.027,P=0.001)。术前低AGR水平患者无复发生存率和无进展生存率较术前高AGR水平患者均明显降低(均P < 0.05)。logistic回归分析显示,高病理分级、高临床分期、肿瘤多发、IMP3阳性、术前低AGR水平均为NMIBC患者预后的危险因素。结论 IMP3蛋白的表达在膀胱癌组织中明显高于癌旁正常组织,低AGR的NMIBC患者肿瘤复发和进展率较高AGR患者的更高,高病理分级、高临床分期、肿瘤多发、IMP3阳性、术前低AGR水平均为影响NMIBC患者预后的危险因素。
-
关键词:
- 非肌层浸润性膀胱癌 /
- 经尿道钬激光切除术 /
- IMP3 /
- 血清白蛋白/球蛋白比值
Abstract: Objective To investigate the prognostic value of insulin-like growth factor Ⅱ mRNA binding protein 3 (IMP3) and preoperative serum albumin/globulin ratio (AGR) in patients with non-muscular invasive bladder cancer (NMIBC) after holmium laser transurethral resection (HOLTUR).Methods A total of 146 patients with NMIBC admitted to our hospital from January to December 2016 were selected. Serum AGR was detected before surgery, and IMP3 expression was detected in cancer tissues and adjacent normal tissues. All patients were followed up for five years, and postoperative complications were observed. Clinical characteristics and prognosis in patients with different IMP3 levels were compared. The prognostic value of AGR was analyzed by ROC curve and Kaplan-Meier survival curve, and the risk factors of poor prognosis were analyzed by logistic regression.Results The overall incidence of complications after HOLTUR was 3.42%. The positive expression rate of IMP3 in cancer tissues was 67.12% (98/146), and there was no positive expression of IMP3 in normal adjacent tissues. There were statistically significant differences in histological grade, clinical stage and recurrence in patients with different IMP3 expression levels(all P < 0.05). The 5-year survival rate in patients with IMP3 positive expression in cancer tissues was significantly lower than that in patients with IMP3 negative expression(31.63% vs 60.42%, χ2=11.027, P=0.001). The recurrence-free survival rate and progression-free survival rate of patients with low preoperative AGR level were significantly lower than those with high preoperative AGR level(all P < 0.05). Logistic regression analysis showed that high pathological grade, high clinical stage, multiple tumors, positive IMP3 and low preoperative AGR level were all risk factors of prognosis.Conclusion The expression of IMP3 in bladder cancer tissues is significantly higher than that in adjacent normal tissues. NMIBC patients with low AGR have higher tumor recurrence and progression rates and AGR is higher. High pathological grade, high clinical stage, multiple tumors, positive IMP3 and low preoperative AGR level are all risk factors affecting the prognosis of NMIBC patients. -

-
表 1 不同IMP3表达水平患者临床特征
例(%) 因素 IMP3弱阳性(51例) IMP3强阳性(47例) IMP3阴性(48例) χ2 P 性别 1.125 0.289 男 35(68.63) 29(61.70) 27(56.25) 女 16(31.37) 18(38.30) 21(43.75) 年龄 0.681 0.409 ≤60岁 17(33.33) 16(34.04) 19(39.58) >60岁 34(66.67) 31(65.96) 29(60.42) 肿瘤直径 2.447 0.118 ≤3 cm 35(68.63) 33(70.21) 27(56.25) >3 cm 16(31.37) 14(29.79) 21(43.75) 肿瘤病发情况 6.173 0.013 单发 28(54.90) 18(38.30) 33(68.75) 多发 23(45.10) 29(61.70) 15(31.25) 病理组织分级 18.143 < 0.001 G1 14(27.45) 12(25.53) 22(45.83) G2 26(50.98) 13(27.66) 25(52.08) G3 11(21.57) 22(46.81) 1(2.09) 临床分期 6.659 0.010 Ta 13(25.49) 9(19.15) 17(35.42) T1 25(49.02) 14(29.79) 23(47.92) T2~T4 13(25.49) 24(51.06) 8(16.66) 复发情况 23.368 < 0.001 复发 34(66.67) 41(87.23) 17(35.42) 未复发 17(33.33) 6(12.77) 31(64.58) 表 2 影响NMIBC患者预后的危险因素
因素 B S.E. Wald P OR 95%CI 病理分级高 2.114 0.425 4.532 0.002 1.234 1.034~2.695 临床分期高 2.231 0.617 4.815 0.008 1.156 1.127~2.889 多发性肿瘤 1.742 0.704 5.346 0.005 1.478 1.076~4.116 IMP3阳性 2.005 0.663 4.471 0.010 1.729 1.247~6.973 术前低AGR水平 1.946 0.741 5.134 0.004 1.774 1.397~6.756 -
[1] 王振誉, 朱华, 张冰, 等. 经尿道钬激光整块切除术治疗非肌层浸润性膀胱癌的疗效分析[J]. 临床泌尿外科杂志, 2021, 36(10): 789-791, 795. https://www.cnki.com.cn/Article/CJFDTOTAL-LCMW202110007.htm
[2] Kardoust Parizi M, Enikeev D, Glybochko PV, et al. Prognostic value of T1 substaging on oncological outcomes in patients with non-muscle-invasive bladder urothelial carcinoma: a systematic literature review and meta-analysis[J]. World J Urol, 2020, 38(6): 1437-1449. doi: 10.1007/s00345-019-02936-y
[3] Fadaak K, Al-Otaibi A, Al-Zahrani A, et al. Transurethral Resection for the Treatment of an Inflammatory Myofibroblastic Tumor of the Urinary Bladder: A Case Report[J]. Case Rep Oncol, 2019, 12(2): 344-353. doi: 10.1159/000500503
[4] Shah A, Tan WP, Inman BA. National Quality Improvement Program in Transurethral Resection of Bladder Tumor: A Model for the Rest of Us, Even if We Cannot Share All Results[J]. Eur Urol, 2020, 78(4): 531-532. doi: 10.1016/j.eururo.2020.07.020
[5] 周强, 杨飞亚, 邢念增. 胰岛素样生长因子Ⅱ mRNA结合蛋白3表达与非肌层浸润性膀胱癌预后的相关性研究[J]. 中华泌尿外科杂志, 2017, 38(8): 586-590. doi: 10.3760/cma.j.issn.1000-6702.2017.08.007
[6] Dougaz W, Bouasker I, Gouta EL, et al. Predictive factor of recurrence after curative resection for stage Ⅰ-Ⅱ colon cancer[J]. Tunis Med, 2019, 97(5): 685-691.
[7] 中华医学会病理学分会泌尿与男性生殖系统疾病病理专家组. 膀胱癌标本规范化处理和病理诊断共识[J]. 中华病理学杂志, 2020, 49(4): 305-310. doi: 10.3760/cma.j.cn112151-20190620-00358
[8] 王小刚, 刘强, 王伯栋, 等. 人脑胶质瘤组织的IMP3和IGF2的表达水平及其临床意义[J]. 临床和实验医学杂志, 2019, 18(19): 2063-2066. doi: 10.3969/j.issn.1671-4695.2019.19.014
[9] 黄健, 刘皓. 非肌层浸润性膀胱癌的诊治现状与对策[J]. 中华泌尿外科杂志, 2019, 40(7): 481-484. doi: 10.3760/cma.j.issn.1000-6702.2019.07.001
[10] 赵色玲, 刘焜, 陈水兰, 等. 经尿道钬激光膀胱肿瘤整块切除术与经尿道膀胱肿瘤电切术治疗非肌层浸润性膀胱癌的对比研究[J]. 国际泌尿系统杂志, 2021, 41(3): 411-415. doi: 10.3760/cma.j.cn431460-20191104-00008
[11] 谭健秋, 黄秋宝, 冯能贵, 等. 经尿道1470 nm激光切除术与TURis治疗非肌层浸润性膀胱癌的疗效比较[J]. 临床医学工程, 2019, 26(7): 881-882. doi: 10.3969/j.issn.1674-4659.2019.07.0881
[12] Das A, Cohen JE, Ko OS, et al. Surgeon Scorecards Improve Muscle Sampling on Transurethral Resection of Bladder Tumor and Recurrence Outcomes in Patients with Nonmuscle Invasive Bladder Cancer[J]. J Urol, 2021, 205(3): 693-700. doi: 10.1097/JU.0000000000001372
[13] 段晓波, 代庆德, 周婷婷. 非肌层浸润性膀胱癌采用两种TURBT术治疗的效果及预后对比研究[J]. 临床和实验医学杂志, 2020, 19(12): 1322-1325. doi: 10.3969/j.issn.1671-4695.2020.12.026
[14] Palou-Redorta J, Solsona E, Angulo J, et al. Estudio retrospectivo de diferentes opciones de tratamiento conservador con Bacilo de Calmette-Guèrin en el carcinoma urotelial vesical T1G3: terapia de mantenimiento[J]. Actas Urológicas Espaolas, 2016, 3(2): 370-377.
[15] 王善龙, 贺利明, 张永升, 等. 经尿道钬激光切除术与等离子电切术治疗非肌层浸润性膀胱肿瘤的疗效及安全性对比[J]. 实用癌症杂志, 2017, 32(8): 1345-1347. doi: 10.3969/j.issn.1001-5930.2017.08.037
[16] 胡洋洋, 牛晓振, 王光春, 等. 2 μm激光、钬激光和经尿道膀胱肿瘤切除术治疗非肌层浸润性膀胱癌的比较研究[J]. 临床与病理杂志, 2016, 36(4): 444-449. https://www.cnki.com.cn/Article/CJFDTOTAL-WYSB201604019.htm
[17] 张宁, 艾斯卡尔, 胡晓刚, 等. 非肌层浸润性膀胱癌2种术式的比较[J]. 中国微创外科杂志, 2017, 17(7): 599-601. doi: 10.3969/j.issn.1009-6604.2017.07.006
[18] Kim JK, Jeong CW, Kwak C, et al. Progression to T1 High Grade(T1HG)from a Lower Stage/Grade is Associated with Poorer Survival Outcomes than Initial Diagnosis with T1HG Bladder Cancer[J]. Ann Surg Oncol, 2017, 24(8): 2413-2419. doi: 10.1245/s10434-017-5902-7
[19] 张玥, 李飞, 杨帆, 等. 术前血清白蛋白水平对非肌层浸润性膀胱癌患者行经尿道膀胱肿瘤电切术的预后价值[J]. 南方医科大学学报, 2018, 38(2): 192-197. https://www.cnki.com.cn/Article/CJFDTOTAL-DYJD201802013.htm
[20] 高超, 蒋林君, 毛明焕, 等. 不同分期膀胱癌患者白蛋白与球蛋白比值的临床意义[J]. 中国医科大学学报, 2021, 50(9): 833-837. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGYK202109014.htm
[21] 李峰, 冯宇鹏, 连学雄, 等. 膀胱癌组织前梯度蛋白2表达变化及其临床意义[J]. 山东医药, 2018, 58(20): 60-62. https://www.cnki.com.cn/Article/CJFDTOTAL-SDYY201820020.htm
-




 下载:
下载: