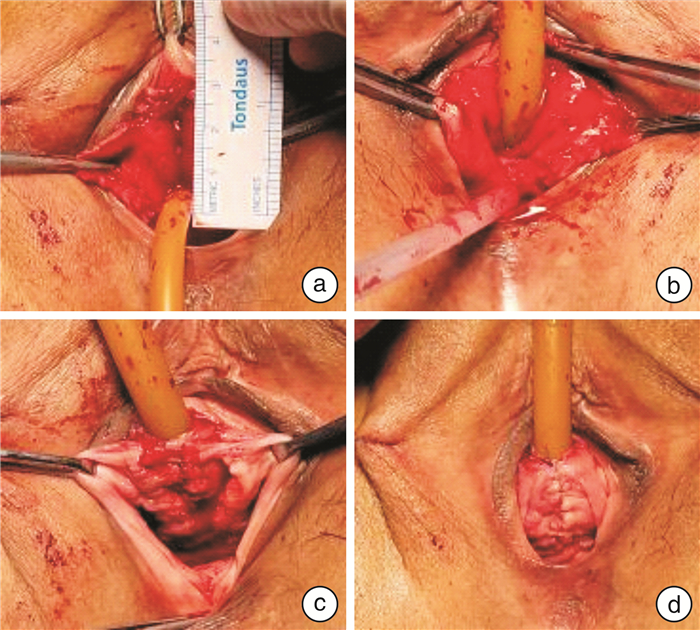
Evaluation of the efficacy of one-stage reconstruction after total urethrectomy for female urethral cancer
-
摘要: 目的 观察并评估尿道癌全尿道切除术后一期行尿道重建术后控尿及预后情况。方法 回顾性分析2018—2020年21例女性患者行全尿道切除加一期尿道重建手术后随访2年尿道镜检查、尿垫实验、残余尿监测的临床资料,评估患者复发预后情况及控尿情况。结果 术后3、6、12、18、24个月定期复查。21例患者膀胱软镜检尿道狭窄评分为(3.52±0.13)分,主观主诉无尿失禁症状。1 h尿垫实验为(1.27±0.32) g。泌尿系超声均未发现患者有肾积水、输尿管扩张、残余尿等情况。腹股沟淋巴结超声均未见明显肿大淋巴结。术后6、12、18、24个月盆腔MRI均未见膀胱壁、尿道异常增厚等情况。显示肿瘤控制良好,预后佳,2年内均无复发,患者对于控尿情况均满意。结论 尿道肿瘤患者给予保留膀胱全尿道切除并行一期重建吻合术后肿瘤根治性切除效果佳,控尿情况良好,临床安全可靠值得应用及推广。Abstract: Objective To observe and evaluate urinary control and prognosis after one-stage urethral reconstruction after total urethrectomy for urethral cancer.Methods We retrospectively analyzed the clinical data of 21 female patients who underwent total urethrectomy and primary urethral reconstruction surgery from 2018 to 2020. Urethroscopy, urine pad test, and residual urine monitoring were followed up for two years. The patient's recurrence, prognosis and urinary control status were assessed.Results Patients were regularly followed up at 3, 6, 12, 18, and 24 months after surgery. The score of urethral stricture on bladder soft endoscopy in 21 patients was (3.52±0.13). No urinary incontinence was in subjective complaint. One-hour urine pad test was (1.27±0.32) g. Urinary ultrasound did not record patients with hydronephrosis, ureteral dilation, or residual urine. Ultrasound showed no obvious enlarged lymph nodes in the inguinal lymph nodes. At 6, 12, 18, and 24 months after surgery, there was no abnormal thickening of the bladder wall or urethra on pelvic MRI. The tumor was well controlled and the prognosis was good. There was no recurrence within two years, and the patient's urinary control was satisfactory.Conclusion Patients with urethral tumors who underwent bladder sparing total urethrectomy combined with one-stage reconstruction and anastomosis have achieved good results in urinary control, and clinical safety and reliability, so this surgical procedure is worthy of application and promotion.
-

-
[1] Chang SS. Urologic oncology: bladder, penis, and urethral cancer, and basic principles of oncology[J]. J Urol, 2023: 101097JU0000000000003735. doi: 10.1097/JU.0000000000003735
[2] Ortac M, Ekerhult TO, Zhao WX, et al. Tissue engineering graft for urethral reconstruction: is it ready for clinical application?[J]. Urol Res Pract, 2023, 49(1): 11-18. doi: 10.5152/tud.2023.22226
[3] 李惠珍, 刘智勇, 王磊, 等. 会阴环形皮瓣在女性尿道口癌控尿性前尿道缺失一期吻合中的应用[J]. 第二军医大学学报, 2017, 38(4): 511-514.
[4] Ishikawa K, Nagata M, Anno Y, et al. Successful wound closure using fibrin glue for intractable neobladder-urethral anastomosis leakage after radical cystectomy and neobladder reconstruction[J]. IJU Case Rep, 2023, 6(5): 267-270. doi: 10.1002/iju5.12592
[5] Elliott SP. Trauma, and genital and urethral reconstruction[J]. J Urol, 2023: 101097JU0000000000003690. doi: 10.1097/JU.0000000000003690
[6] Borgognone A, Santi GD, Baffigo G, et al. Is a pedicular flap coupled to the double turnover flaps urethroplasty suitable for urethral-perineal reconstruction? Considerations about a relapsing urethral-cutaneous fistula condition[J]. JPRAS Open, 2023, 38: 91-97. doi: 10.1016/j.jpra.2023.08.002
[7] Jamil ML, Hamsa A, Grove S, et al. Outcomes of urethroplasty for synchronous anterior urethral stricture utilizing the trauma and urologic reconstruction network of surgeons length, segment and etiology anterior urethral stricture classification system[J]. Urology, 2023, 181: 155-161. doi: 10.1016/j.urology.2023.08.017
-




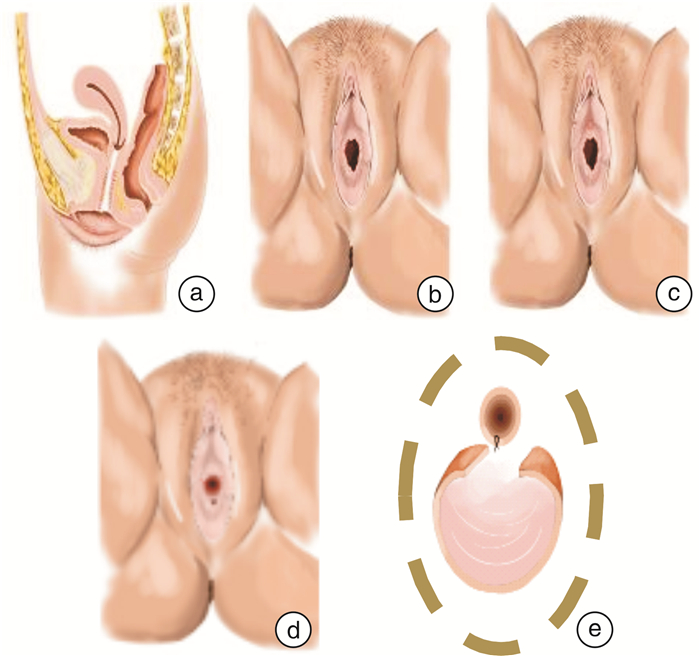
 下载:
下载: